Preventing Pressure Injury in Prone Positioning
Prone positioning, which involves turning a patient over so that they lie in a chest-down, is a well-established intervention for ARDS. It has been shown to improve oxygenation and prevent ventilator-induced lung injury due to the more uniform distribution of lung stress and strain1,2.
While prone positioning, or lying the patient face-down (see Fig. 1), has been recommended since as far back as 19743 for treating ARDS, the recent COVID-19 pandemic has driven an increase in the necessity for and utilisation of prone positioning as a method to improve life-threatening low oxygen levels.
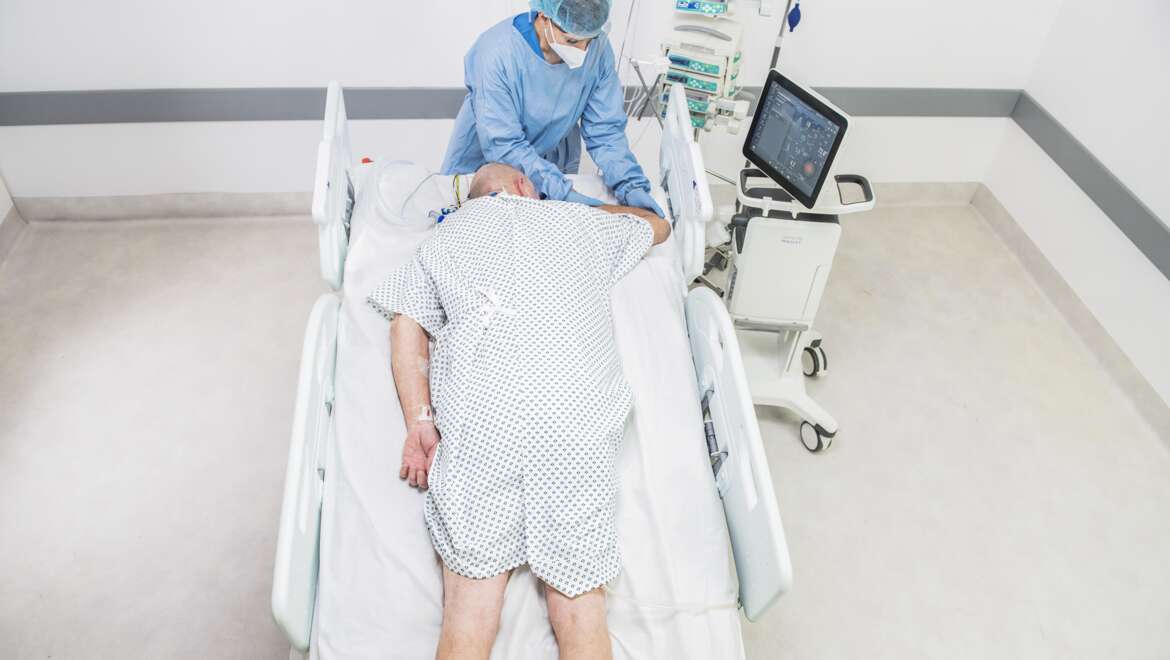
Figure 1: A patient in prone position.
The latest guidelines4 suggest that prone sessions should last for more than 16 hours each day to take advantage of physiological changes that can result in improved oxygenation.
However, managing patients in the prone position for such prolonged periods places the patients at significant risk of complications, including pressure injury5. Such injuries can lead to a protracted hospital stay, patient suffering, possible surgical intervention, and increased costs of care6.
When caring for patients in the prone position, caregivers are challenged to prevent pressure injuries developing over body areas such as the face, breast region, genitals, knees and toes (Fig. 2), not typically at risk when the patient is managed supine, but at high risk when patients are in the prone position.
_Blog%20Image.jpg)
Figure 2: Areas of the body subjected to higher pressure when in prone position.
Selecting the right support surface is therefore an important component to be deployed with this high risk patient population.
The Nimbus Professional alternating pressure mattress replacement system includes ‘Zoned wound valve technology’ (Fig. 3 and 4), designed to specifically help off-load vulnerable body areas, providing an appropriate support surface solution when prone positioning is required.
This enables the caregiver to off-load selected cells under the under parts of the body at specific risk, while the head section can be deflated to give flexibility to caregivers in managing the patients head and airway.

Figure 3: Wound valves along the full length of the Nimbus Professional support surface allow specific cells to be deflated in order to offload pressure.
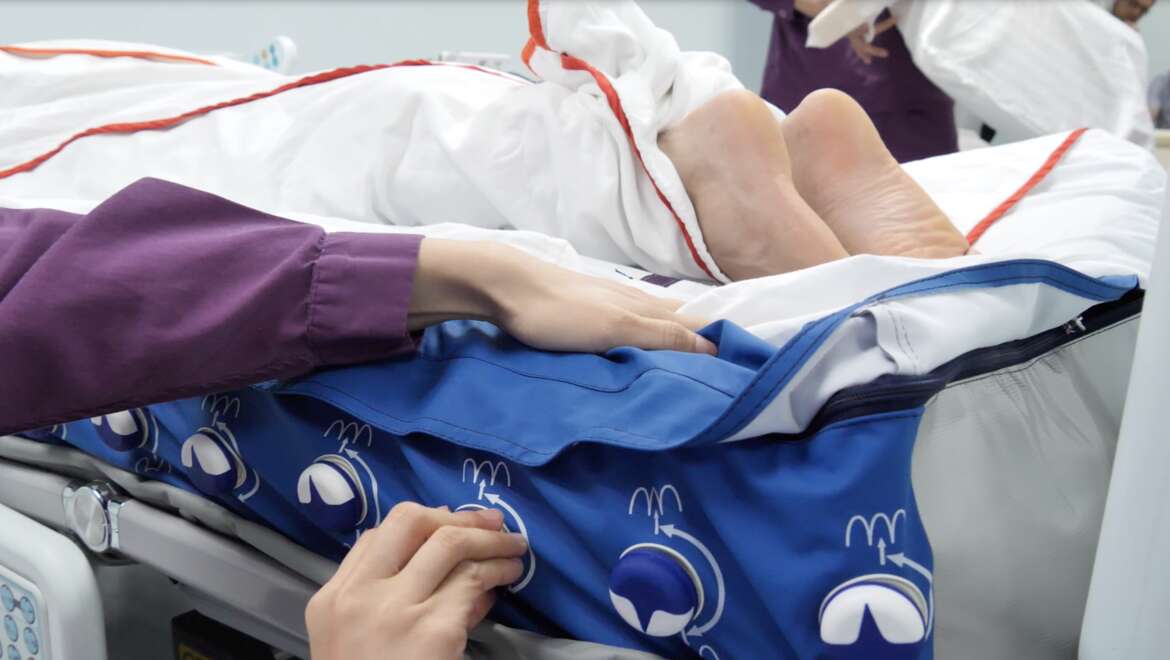
Figure 4: Adjusting the Wound Valves on a Nimbus Professional.
The Nimbus Professional mattress also offers the additional benefit of a fully-welded cover constructed from one of the toughest medical fabrics available7.
Extensive clinical studies8-15 on the Nimbus product range consistently demonstrate excellent outcomes for the most vulnerable patients or those with existing wounds.
Explore our Prone Positioning Solutions page or visit the Nimbus Professional page to learn more.
References
- Dardeir A, Marudhai S, Patel M, Ghani MR, Busa V. Factors Influencing Prone Positioning in Treating Acute Respiratory Distress Syndrome and the Effect on Mortality Rate. Cureus. 2020 Oct 2;12(10):e10767. doi: 10.7759/cureus.10767. PMID: 33033667; PMCID: PMC7532878.
- Koulouras V, Papathanakos G, Papathanasiou A, Nakos G. Efficacy of prone position in acute respiratory distress syndrome patients: A pathophysiology-based review. World J Crit Care Med. 2016 May 4;5(2):121-36. doi: 10.5492/wjccm.v5.i2.121. PMID: 27152255; PMCID: PMC4848155.
- Bryan AC, Conference on the scientific basis of respiratory therapy. Pulmonary physiotherapy in the pediatric age group. Comments of a devil’s advocate. Am Rev Respir Dis 1974; 110: 143–144.
- Papazian, L, Aubron, C, Brochard, L et al, 2019. Formal guidelines: management of acute respiratory distress syndrome. Annals of Intensive Care, 9(1).
- Girard R, Baboi L, et al The impact of patient positioning on pressure ulcers in patients with severe ARDS: results from a multicentre randomised controlled trial on prone positioning, Intensive Care Med (2014) 40:397–403 4.
- Bunker D, Thomson M, Chin Necrosis as a Consequence of Prone Positioning in the Intensive Care Unit Case Reports in Medicine Volume 2015, Article ID 762956.
- Dartex Coatings Limited, 2013. The Impact of Cleaning Chemicals on Polyurethane Mattress Cover Materials and their Propensity for Physical Damage. Authored by Jo Milnes MA(Hons), MSc(Dist), Technical Manager.
- Ward C, Wubbels M, Schembri L (2012) Using Complete Pressure Off-loading and Advanced Wound Care to Treat a Complex Sacral Pressure Ulcer. Poster Presentation.
- Clancy J (2011) Winning the war against pressure ulcers. Poster presentation.
- Malbrain M, Hendriks B, Wijnands P et al (2010) A pilot randomised controlled trial comparing reactive air and active alternating pressure mattresses in the prevention and treatment of pressure ulcers among medical ICU patients. Journal of Tissue Viability 19(1):7-15.
- Finnegan MJ (2008). Comparing the effectiveness of a specialised alternating air pressure mattress replacement system and an air fluidised integrated bed in the management of post- operative flap patients. A randomised controlled study. Journal of Tissue Viability 17(1): February 2008.
- Russell L, Reynolds TM (2000) Randomised controlled trial of two pressure relieving systems. Journal of Wound Care 9(2):52-55.
- Evans D, Land L, Geary A (2000). A clinical evaluation of the Nimbus 3 alternating pressure mattress replacement system. Journal of Wound Care 9(4):181-186.
- Land L, Evans D, Geary A et al (2000) A clinical evaluation of an alternating pressure mattress replacement system in hospital and residential care settings. Journal of Tissue Viability 10(1): 6-11
- Phillips L (2010) Nimbus range of pressure redistributing mattresses. Wounds UK, 2010, 6 (2): 116-122.



