Rehabilitation through early mobilization after surgery – your guide to helping people recover faster
In the aftermath of the COVID-19 pandemic, healthcare providers around the world are facing huge backlogs of surgeries and treatments. Efforts to shorten recovery times for patients by supporting early mobilization can help to increase the flow of patients in hospitals.
Using assistive patient handling solutions is an efficient way to help regain or maintain mobility – and we are here to support every step on the way. Our Rehabilitation guide helps to empower movement, while reducing the risk of caregiver injuries.
Low physical activity during hospitalization leads to loss of muscle strength, functional performance and independence, so it is obvious that empowering movement in hospitals and care facilities has multiple benefits for patients and residents. Mobility improves dignity, independence, and can lead to improvements in physical and mental wellbeing.
However, helping patients and residents to move also involves major challenges for caregivers. Musculoskeletal injuries continue to be the leading cause of injury in healthcare, with 55-91% of physical therapists estimated to experience work related musculoskeletal disorders (WMSD) and one in six make career changes as a result of injury.1,2
"55-91% of physical therapists estimated to experience work related musculoskeletal disorders.1,2"
The focus on patient fall prevention programmes is another factor that has resulted in unintended consequences for patient mobility, functional ability and well-being.3 Activities have not been encouraged due to the perception that improving mobility also increases the number of falls. However, studies show this perception is false.4
As an example, leaving a patient in a low-bed height was once considered a universal solution to preventing falls. In fact, it isn’t. When the bed is too low, it can act as a passive restraint, and residents can find it difficult or even impossible to get out of bed without help.5
When residents lose the ability to stand up from a sitting position unassisted, their functional independence can go into decline.6
Assistive patient handling technology is your ‘mobility partner’
The use of assistive patient handling solution technology by therapists is supported by best practice guidelines, and actually reduces the risk of hospital acquired harm. During the rehabilitation process, these aids can be seen as a ‘mobility partner’ to facilitate functional mobility, promote patient safety and reduce caregiver injury.1,2,7
Therapists have reported that patient handling equipment increased their options for therapeutic activities and allowed them to mobilise patients earlier in the rehabilitation process compared to not having the equipment available.2
Even if mobilisation and rehabilitation often are seen as activities handled by a therapist, there are also many opportunities for all caregivers to integrate mobility into the daily care work.8
Our guide ‘Rehabilitation through Empowering Movement’ offers guidelines on how to assist and enhance moments for mobility by introducing technology as a supporting aid in the rehabilitation therapy.
With the Arjo Mobility Gallery as a base, our rehabilitation guide describes a number of mobility activities and how these can be facilitated by using assistive technology. Here are some examples of our solutions and the activities they support.
POWERED SIT-TO-STAND
Sara Plus® – powering raising and standing
Sara Plus is a powered standing and raising aid designed for operation by a single caregiver. With a detachable foot plate and the support of an arc rest and sling, Sara Plus facilitates active transfers as well as balance, stepping and gait training.
With the patient sitting on the edge of the bed, Sara Plus supports movements involving varying heights, distances and activities. Sara Plus also encourages the patient to stand and sit independently and engage in functional activities that can help improve static and dynamic balance and weight transfer.
This active lift can also be used out of bed. For example, a patient supported by Sara Plus and sitting on a gym ball is able to engage in activities that promote the balance.
In walking situations, supported by the Sara Plus walking sling and the arc rest at correct height for patient support, the footplate can be removed for mobility practice. The patient can safely step through and mobilise by practicing normal movements.
You can also help patients practice independent moves that focus on standing balance and weight bearing tolerance. To do this, place the patient on an upright position using the Sara Plus to encourage them to stand away from the support of the sling.
NON-POWERED SIT-TO-STAND
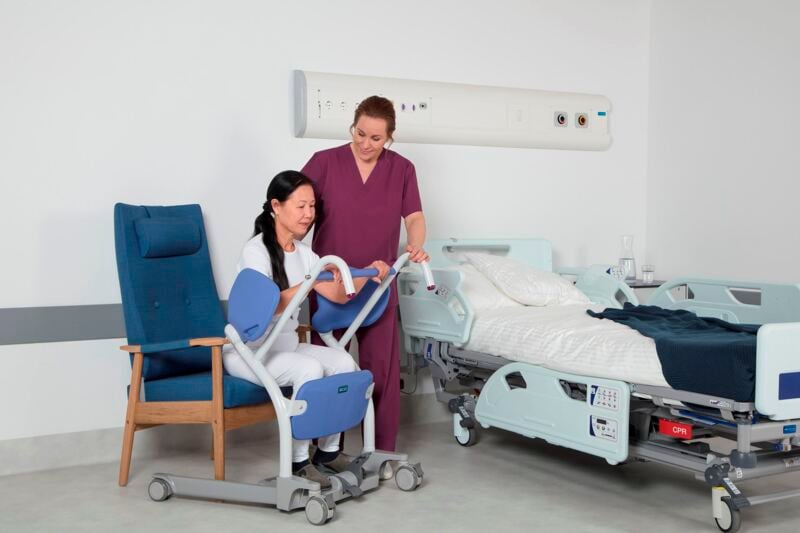
Sara Stedy® – enabling steady sit-to-stand tasks
Sara Stedy is a non-powered device that supports early mobility initiatives by enabling a single caregiver to assist sit-to-stand tasks for patients of different sizes and clinical assessments.
In a perch position, it supports core stability and functional activities. Sara Stedy also encourages the patient to lean forward and initiate the standing movement with concentric lower limb activation and the correct weight transference.
During the pull-up into standing, Sara Stedy supports the activation of the abdominal, thigh and lower limb muscles that bring the hips forward to an upright position.
CEILING LIFT
Maxi Sky® 2 – Ensuring a safe, comfortable and dignified transfers
The Maxi Sky 2 ceiling lift helps a single caregiver to transfer patients or residents smoothly without any manual lifting. This reduces the risk of injury both for the caregiver and the person in the lift.
The Maxi Sky 2 ceiling lift opens up for a number of different activities. Some examples:
Using a repositioning sling in combination with a passive lift can help reduce the impact on the caregiver workflow when rolling and turning a patient in bed.⁹
Seated activities at the edge of the bed or out of bed are also facilitated. Using the ceiling lift with an ambulation sling, combined with a walking frame, can offer additional support and confidence when practising walking. This allows the therapist to focus on guiding the activity, while ensuring a correct use of the mobility aid.
Training how to recover from a fall is an important step to enable self-management when the patient returns home. These activities can be enabled by using a ceiling lift and an ambulation sling. The therapist is able to guide the patient to sitting or standing by following a normal movement pattern.
Activities in daily life are meaningful to individuals and an important part of rehabilitation programmes. However, these activities can be difficult to practice without additional support. By ensuring that the patients’ feet are on the floor to support normal patterns of movement, the ceiling lift can help improve static and dynamic standing balance, weight bearing and gait activities.
A partnership that empowers mobility
All Arjo solutions are based on our dedication to support therapists’ fundamental aim of empowering mobility and restoring the quality of patients’ and residents’ lives.
We work in partnership with you to find solutions that can help achieve therapeutic goals and activities, while also reducing the risk of musculoskeletal injury that can be associated with many physical therapy interventions. The Arjo consultancy programs such as Arjo Move are designed to provide the healthcare facility with positive and measurable quality, clinical, operational and financial outcomes. A partnership with us paves the way for unlocking potential and a sustainable culture that fine tunes existing processes and efficiencies for improved patient outcomes, staff wellbeing and financial optimisation.
Reference list
1. Daragh A, et al. Safe Patient Handling Equipment in Therapy Practice: Implications for Rehabilitation. The American Journal of Occupational Therapy. 2013; 67(1):45-53.)
2. Cromie JE, Robertson VJ, Best MO: Work-related musculoskeletal disorders in physical therapists: prevalence, severity, risks, and responses. PhysTher 2000, 80(4):336-351. 3. https://www.who.int/disabilities/care/rehabilitation_guidelines_concept. pdf Accessed 15-10-2020
4. JAMA Intern Med. 2017 June 01; 177(6): 759–760
5. Haines, T.P., Bell, R.A. and Varghese, P.N. (2010), Pragmatic, Cluster Randomized Trial of a Policy to Introduce Low-Low Beds to Hospital Wards for the Prevention of Falls and Fall Injuries. Journal of the American Geriatrics Society, 58: 435-441.
6. Hughes, M. A., Schenkman, M. L. (1996). Chair rise strategy in the functionally impaired elderly. Journal of Rehabilitation Research & Development, 33(4), 409-412.
7. European Pressure Ulcer Advisory Panel, National Pressure Injury Advisory Panel and Pan Pacific Pressure Injury Alliance. Prevention and Treatment of Pressure Ulcers/Injuries: Clinical Practice Guideline. The International Guideline, Emily Haesler (Ed.)EPUAP/NPIAP/PPIA:2019. Section 8: Repositioning and Early Mobilisation Recommendation 5.6 Repositioning Techniques. Page 121
8. Alzheimer's Society of Canada (2020)
9. Wiggerman N., Zhou J., McGann N. (2020). Effect of repositioning aids and patient weight on biomechanical stresses when repositioning patients in bed, 2020. https://doi.org/10.1177/0018720819895850. Accessed 15-10-2020








