Latest

Safe patient handling, Mobility
Feb 27, 2025
‘Microclimate Does Matter’ – Analysis of RCT-based Results for At-Risk Patients
(-EUR ING David NewtonA,C M.Eng, C.Eng, MIET, MIEEE, Sara TacksonB,C PT, MPT, CWS)
A pressure injury (PI) results in adverse clinical impact for patients and staff along with increased financial burden to the healthcare facility, potential litigation costs1, and additional federal reporting implications2

Safe patient handling, Mobility
Feb 27, 2025
‘Remaining Tough Under Pressure’ – Support Surface Covers in the Post-Pandemic World
(-EUR ING Dave NewtonA,C,D, M.Eng, C.Eng, MIET, MIEEE, Richard HaxbyB,C,D, BSc (Hons) Ebor)
Support surface contamination via ingress through the cover material has long been a concern.
Safe patient handling, Mobility
Feb 27, 2025
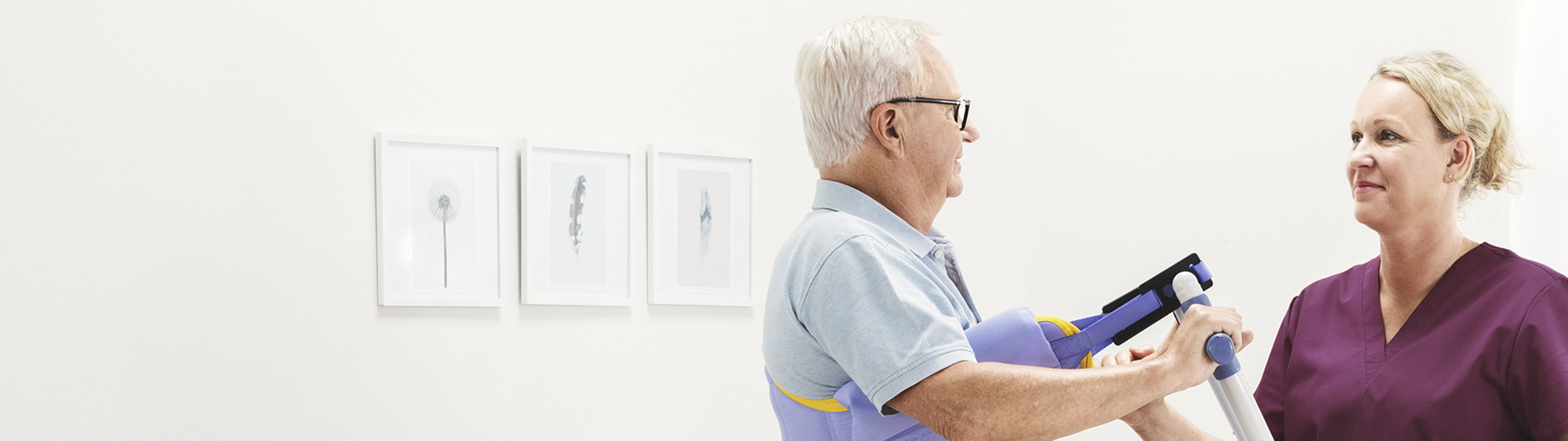
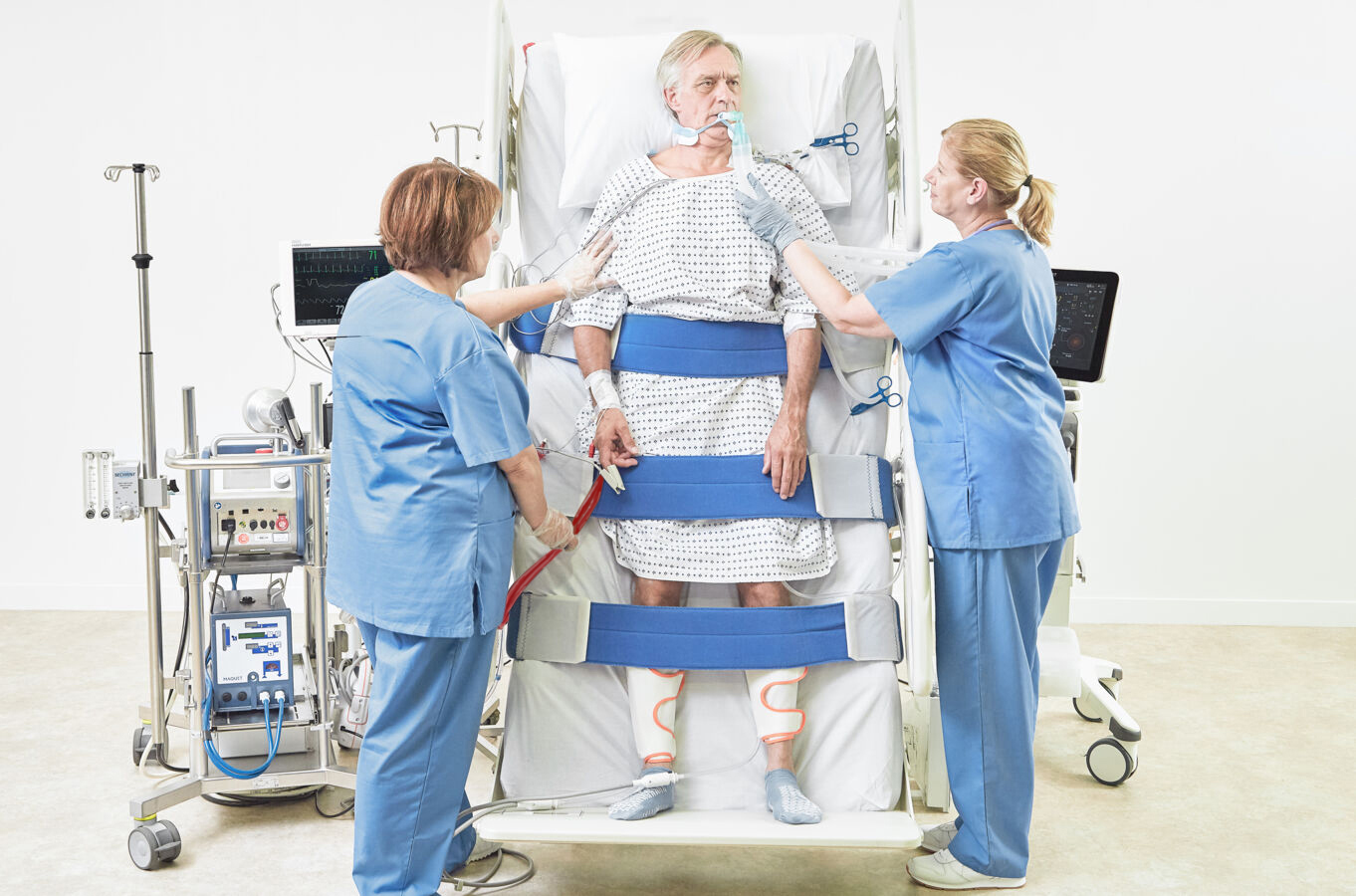
’Reduce the pressure and don’t sweat it!’ – Verticalization Therapy
(-Sharon Maris RN, Dominic Baily MIET, Carroll Gillespie RN, BSN, MS, CWOCN)
In critically ill patients, prolonged bed rest and immobility can lead to severe physical deconditioning, significant loss of muscle mass, and increased muscle weakness1. Verticalization therapy is utilized as a component of early critical care recovery protocols.

Early Mobility
Jan 14, 2025
Addressing the Devastating Effects of Immobility with the Sara Combilizer
Immobility causes devastating effects on a patient, whether they’re in the ICU or any other unit of a hospital.

Early Mobility
Jan 14, 2025
Essential Attributes of the Sara Combilizer: Enhancing Patient Mobility and Safety
Early mobilization has been demonstrated to be both safe and feasible for patients admitted to critical care.

Early Mobility
Jan 14, 2025
Optimizing Patient Care with the Sara Combilizer - Practical Tips and Real-World Clinical Applications
Where edge of bed sitting is likely to be difficult to achieve, but early weight bearing and upright positioning are desirable, the Sara Combilizer a multiposition aid can be utilized to help achieve out of bed rehabilitation goals early in the care pathway.

Pressure injury prevention
Oct 22, 2024
The power of intervention in pressure injury prevention and management
by Sharon Maris, Director Global Medical Affairs for Pressure Injury Prevention
Pressure injury prevention interventions are key to reducing the risk of developing painful, resource intensive and costly pressure injuries.

Early Mobility
Oct 08, 2024
Enhancing the Veteran’s Journey: A Deep Dive into Arjo's Veterans Mobility Gallery
Arjo is proud to introduce the Veterans Mobility Gallery, an initiative that reflects our commitment to supporting the Veterans Affairs Administration. This gallery isn't just a collection of stories; it's a homage to the courage, resilience, and diverse needs of our veterans from all branches of the military — Marine Corps, Air Force, Navy, Army, and the Coast guard — illustrated through the personalized mobility journeys of five representative characters.

Medical beds
Sep 06, 2024
Therapeutic Seating Solutions by Arjo: Transforming Care at Holy Angels
We recently had the pleasure of interviewing Paula Atkins, the Chief Clinical Officer at Holy Angels, to discuss the transformative impact of our therapeutic seating solutions on their residents.

Work related injuries, Mobility
Aug 14, 2024
From bedside to bottom line – The guaranteed financial outcome with Arjo MOVE® program
Arjo MOVE program has a proven track record of positively impacting clinical, operational and financial outcomes at healthcare facilities across the US. Our programs create a momentum for change, empowering you to sustain the results long after the end of the program.

Mobility, Work related injuries
Aug 14, 2024
Costs of caregivers’ compensation, treatment of pressure injuries and patient falls in US healthcare facilities
How do we guarantee financial outcomes with Arjo MOVE® Program?
Patient mobilization is not just a clinical priority, but a financial one. Compromised mobility is a widely recognized risk factor for a number of Hospital-Acquired Conditions (HACs). In addition, patients with compromised mobility are more dependent, adding to the burden on caregivers while exposing them to increased risk of physical strain.
Here are some key figures on caregivers’ compensation, treatment of pressure injuries and patient falls in US healthcare facilities:

Safe patient handling, Mobility
Aug 14, 2024
Kern County Hospital Authority - Arjo MOVE® Program
Safe patient handling, progressive mobility, pressure injury prevention and the key role of AirPal®
Kern Medical Center (“Kern Medical”), owned and operated by the Kern County Hospital Authority, is an acute care teaching center with 222 beds offering the only advanced trauma care between Fresno and Los Angeles, California. Kern Medical’s role as a safety net, public hospital places value on innovation adaptability. As a topflight regional health care system, Kern Medical is a leading voice for health, healing and wellness in the Central Valley.

Work related injuries, Mobility
Aug 14, 2024
West Virginia University Hospitals, Inc. - Arjo MOVE® Program
West Virginia University Hospitals, Inc., (Ruby Memorial Hospital), is located in Morgantown, West Virginia & currently has 754 beds with an average of 7,289 employees. We are a level one trauma center and belong to the largest health system in West Virginia.

Work related injuries, Mobility
Aug 13, 2024
UnityPoint Health Methodist - Arjo MOVE® Program
UnityPoint Health Methodist (UPHM) has always striven to deliver for its patients and staff and sought to do so efficiently, advancing its quality of care in concert with reducing staff injuries and cost.

Mobility, Work related injuries
Aug 13, 2024
AnMed Health Case Study - Arjo MOVE® Program
A 98% decrease in workers’ compensation costs and an 82% decrease in patient handling-related injuries helped AnMed Health earn nearly $2.6 million in total annual savings.1

Mobility, Work related injuries
Aug 13, 2024
Adventist Health Sonora Case Study - Arjo MOVE® Program
Adventist Health Sonora is a community medical center that has a vision to transform the health experience of its community by improving health, enhancing interactions, and making care more accessible. This vision also includes the health and well-being of all of its employees.

Work related injuries, Mobility
Aug 13, 2024
Mercy Health Case Study - Arjo MOVE® Program
Arjo MOVE helped Mercy Health save over $2 million1 in the first year.

Work related injuries, Mobility
Aug 13, 2024
Baptist Memorial Health Care - Arjo MOVE® Program
Arjo MOVE helped Baptist Memorial reduce staff injuries by 80 percent on average across their large system of hospitals.
_Blog%20Image_PNG.png)
Microclimate management
Aug 05, 2024
The “Humiditure” is Rising: Dealing with Microclimate in pressure injury prevention
Author: Carroll Gillespie, RN, CWOCN, Clinical Solutions Manager
Like most of the United States, it seems that summer came early and with a vengeance. All states are experiencing excessively high temperatures, and the humidity has been extremely high. In my hometown of Jacksonville, the weather correspondents refer to the “humiditure”, what the air feels like with the high temperature and humidity combined.

Service
Jun 24, 2024
6 Key benefits of preventive maintenance of medical equipment
Partnering with Arjo’s expert service team provides peace of mind towards ensuring equipment meets FDA compliance standards, while experiencing cost savings and safeguarding patient quality care.

Service
May 28, 2024
Arjo ReNu: a recycling solution that reduces the climate impact of healthcare
Medical consumables comprise a large proportion of the total climate impact of healthcare. As such, recycling solutions provide significant opportunities to reduce emissions.

Dementia
Apr 22, 2024
Enhancing Life with Dementia: Soothing music and gentle motions
Author: Dawn Wiggins, RPN, MSc
Sensory Comforts for Enhancing the Well-being of Individuals with Dementia
Incorporating sensory features into the daily routines of individuals living with dementia can significantly enhance their well-being, especially during potentially stressful situations. For those with dementia, the progression of the disease can often disrupt the normal sensory processing and the ability to make sense of the environment, leading to confusion, anxiety, and a decreased ability to manage daily tasks independently. A chair that offers customizable music and a gentle rocking motion can be a soothing presence, providing comfort and reducing anxiety.
Dementia
Apr 22, 2024
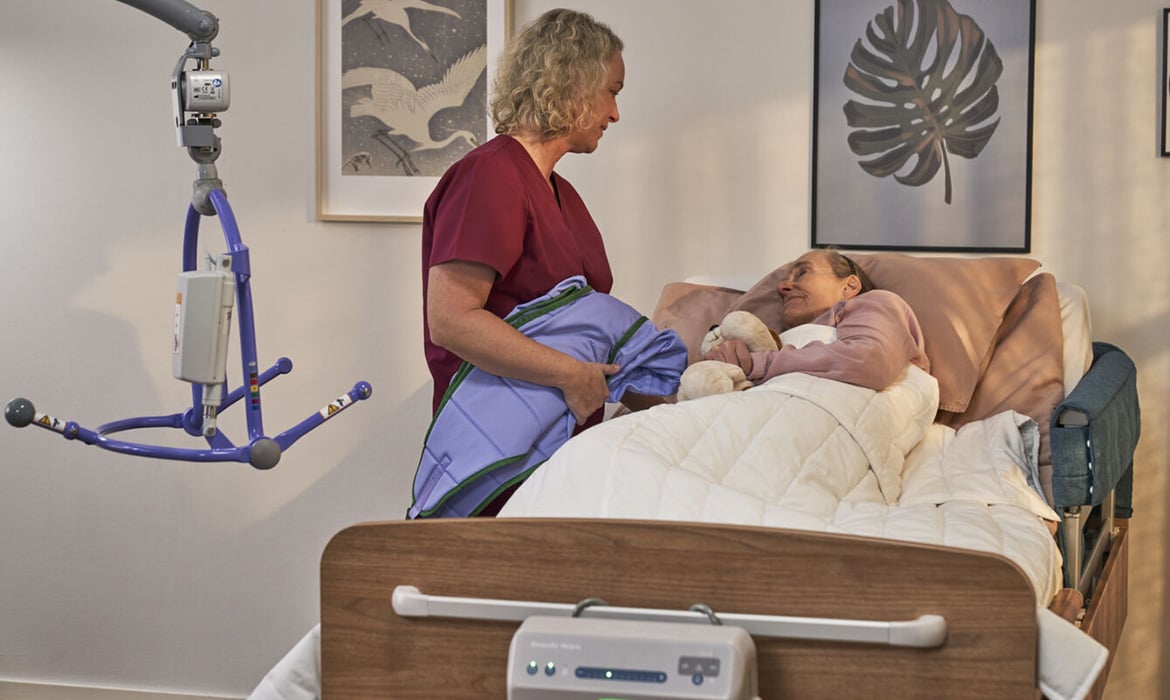
What Are the 7 Domains of Well-Being in Dementia Care?
Author: Dawn Wiggins, RPN, MSc
From Friction to Flow: How the Domains of Well-Being Transform Dementia Care
If you're familiar with the phrase "person-centered care," you'll know it's something of an industry buzzword. But let's get past the jargon and really dig into what it means to offer not just individualized but truly transformative care for people living with dementia. I'm not just talking about sprinkling the term "person-centered" here and there; I'm talking about enriching lives through a focus on the domains of wellbeing.
Dementia
Apr 22, 2024
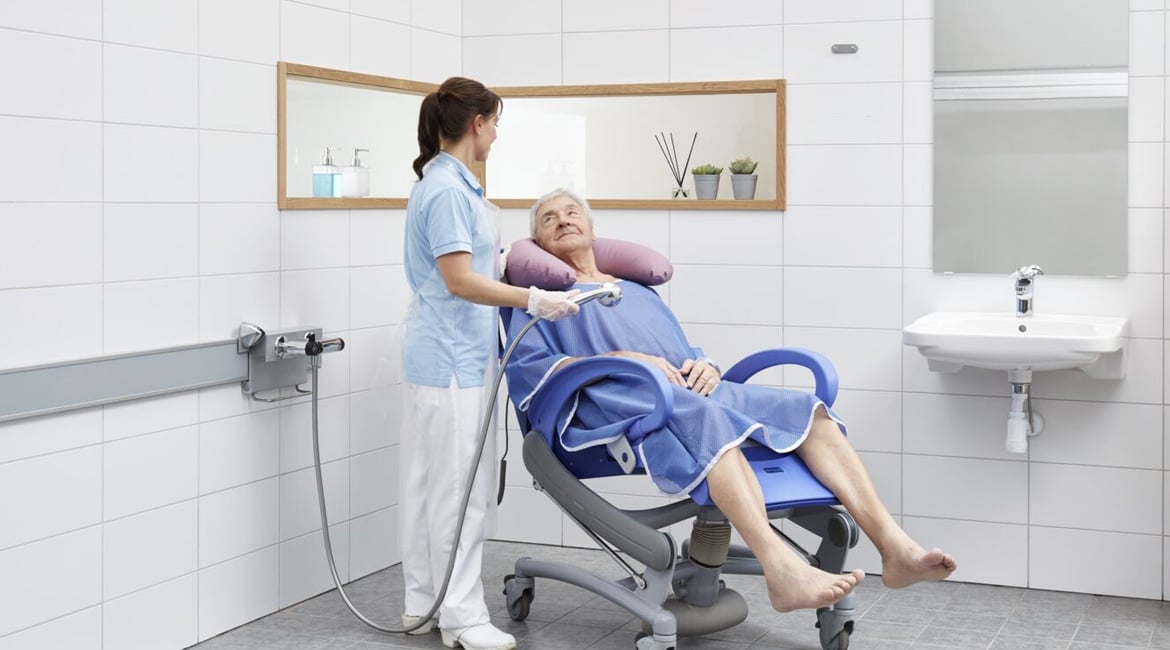
9 Ways Dementia Alters Perception: Adapting Care for Comprehensive Support
Author: Dawn Wiggins, RPN, MSc
Dementia is a complex journey marked by a series of changes that individuals experience as the condition advances. These changes are a natural part of dementia, and comprehending them is crucial for providing effective, person-centered care and purposeful mobility based upon the individual’s optimal level of function.

Dementia
Apr 22, 2024
Empowering Long Term Care Residents: The Role of the Atlanta Chair in Dementia Care Settings
Author: Dawn Wiggins, RPN, MSc
The Atlanta™ chair was accredited with a class 1A rating from the University of Stirling's Dementia and Design Centre, and stands out as a prime example of evidence-based design improving the lives of those with dementia. Addressing both psychological and physical challenges, its features make it a crucial piece of adaptive furniture.

Dementia
Apr 22, 2024
Comfort in Care: Elevating the Experience of Patients Living with Dementia with Thoughtful Design
Author: Dawn Wiggins, RPN, MSc
Every Hour, Every Moment: A Compassionate Approach to Friction-Free Care
In the world of dementia care, the focus is on redefining the caregiving experience with a range of innovative, dementia-accredited products. This holistic approach underscores the importance of relationships in delivering true person-centered care. Understanding that the connections between caregivers and individuals living with dementia are fundamental, this suite of products is designed with features that facilitate and enhance these vital connections, putting the needs and well-being of individuals at the forefront of care.

Pressure injury prevention
Mar 21, 2024
The importance of time in pressure injury development and how Arjo clinical expertise helps improve outcomes
Pressure injuries (PIs) are one of the largest unsolved healthcare challenges today and International pressure injury prevalence rates are estimated to be between 3-32% in Long Term Care facilities.1 Under certain conditions PIs can begin to develop in a matter of minutes to hours2,7. That is why once an individual’s PI risk is assessed and identified, prescribing the right intervention needs to be fast, simple and straightforward.

Medical beds
Mar 19, 2024
The Evenda bed range – designed to help improve life for people living with dementia and their carers

Early Mobility
Feb 21, 2024
The Remarkable Recovery of Matt Rogers: A Testament to Early Mobilization and Human Resilience
In the world of medical miracles, the story of Matt Rogers stands out as a beacon of hope and a testament to the power of modern medicine combined with the human spirit. Matt, a former paramedic and nurse, faced a dire situation when he arrived at the clinic in Georgia, with his health in critical condition. What unfolded next was nothing short of miraculous, as he journeyed back to health and normalcy.

Designing care facilities
Feb 02, 2024
Facility architecture and design in focus: Part 1 – Quality care starts with meticulous planning and decision-making
Part 1 of 5. The foundation for quality care is laid long before the first patients and residents arrive at a healthcare facility. A meticulous approach to architecture and design paves the way for creating comfortable living conditions and an ergonomically sound workplace for the staff. In a series of five articles we are going to highlight the different stages in the architectural process – and their importance for the end result.

Designing care facilities
Feb 02, 2024
Facility architecture and design in focus: Part 2 – Stakeholder interaction: A key factor for resident wellbeing and a sound working environment
Part 2 of 5. The interaction between different stakeholders involved in creating a care facility – such as owners, developers, architects, caregivers and suppliers – is the key to achieving a sound working environment and optimal living conditions for the residents. The second article in this series about design focuses on the architects’ and Arjo’s roles in the process.

Designing care facilities
Feb 02, 2024
Facility architecture and design in focus: Part 3 – Creating space: the main factor in early floor and room planning
Part 3 of 5. When designing a new healthcare facility, space is the factor that stands out as the main enabler for creating comfortable living conditions for residents and a sound working environment for staff. In the third article in this series, we will focus on the importance of meticulous floor and room planning in the early stages of a project.

Designing care facilities
Feb 02, 2024
Facility architecture and design in focus: Part 4 – Elevate assisted bathing to a spa experience with these planning aids
Part 4 of 5. Making the bathing experience homelike and cosy for the resident at the same time as it becomes practical and ergonomically sound for the carers is a challenge that requires a lot of attention in the design process. The fourth article in this series is dedicated to the art of elevating assisted bathing to a spa-like experience.

Designing care facilities
Feb 02, 2024
Facility architecture and design in focus: Part 5 – Optimal care facility creation: understanding the building process
Part 5 of 5. The entire building process of a healthcare facility, from initial study until the first patients or residents arrive, can take five years or even more. Understanding this process is a major enabler for creating a facility that meets all requirements. In the fifth and final article in this series, we take a closer look at the different stages involved.

Dementia
Sep 18, 2023
5 Dementia accredited products that support person-centered care
For those suffering from dementia, the responsive behaviors are among the most distressing and challenging outcomes of the condition. These responsive behaviors most commonly include apathy, depression, irritability, agitation or anxiety. The pressures on a care environment and individual caregivers to mitigate episodes of responsive behavior, as well as the moments of friction they entail, can be significant.
Arjo believes that it is only by applying a person-centered approach when caring for someone living with dementia that quality of life can be maintained, episodes of responsive behavior can be minimized and efficiency can be achieved.1

VTE prevention
Sep 05, 2023
Understanding the Importance of Compression Therapy in VTE Prevention
When we get a small wound, we often praise our blood’s ability to clot to protect the wound and prevent further blood loss. However, when blood starts to clot in the wrong place at the wrong time, the consequences can be life-changing, even fatal. Every year, blood clots in the deep veins cause extensive suffering for millions of people. In this article we’re taking an in-depth look at blood clots, their causes and how the Flowtron Active Compression System can help prevent the condition.
Early Mobility
Jun 27, 2023
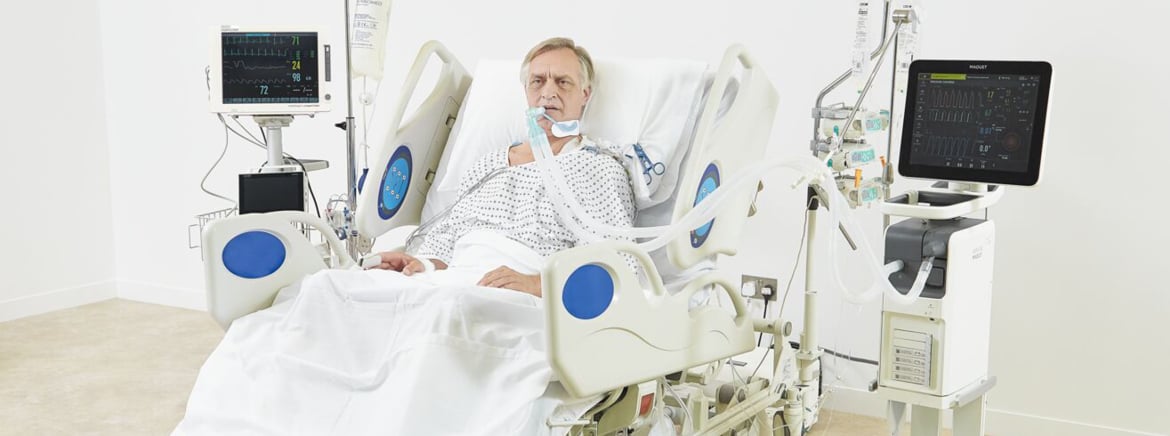
The impact of prolonged immobility & assessment of patient readiness for mobility
Intensive care unit (ICU) patients frequently have extreme derangement of physiological function.
Early Mobility
Jun 27, 2023
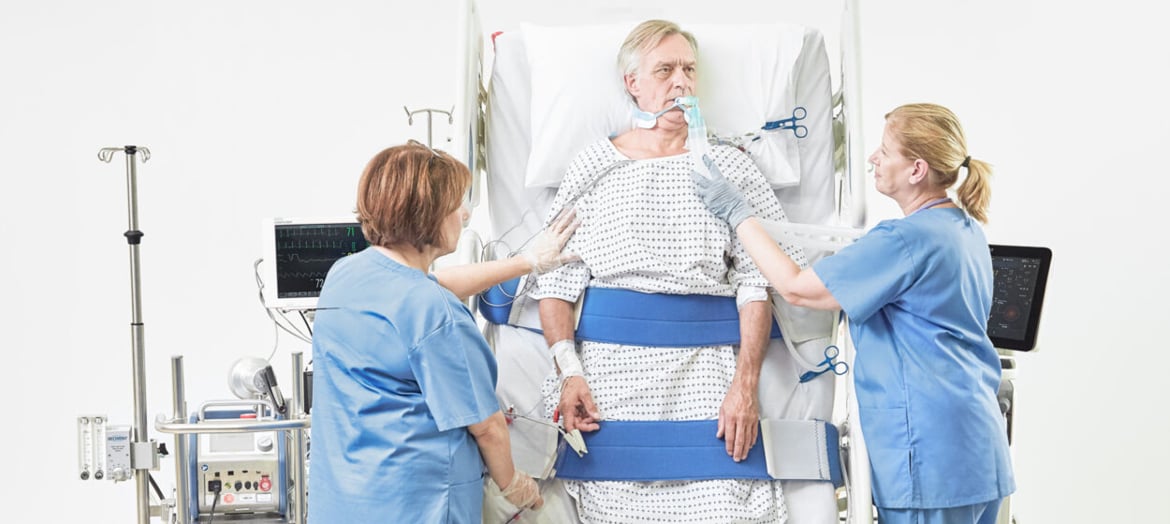
How a lack of assistive equipment can be a barrier to mobility in the ICU
Early mobilization of ICU patients has been associated with improved muscle strength and functional independence, as well as a shorter duration of delirium, mechanical ventilation, and ICU length of stay.1-5
Early Mobility
Jun 27, 2023
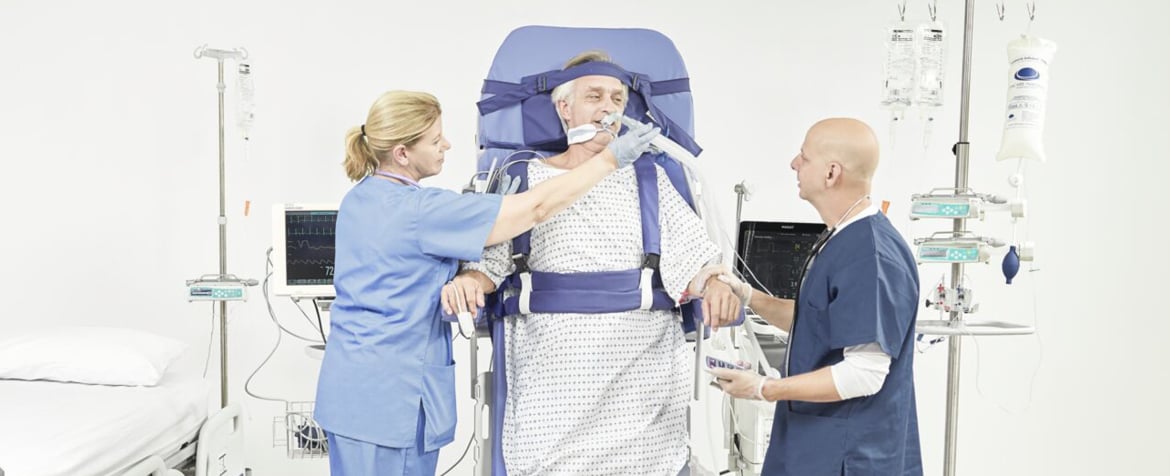
Our early mobility solutions supporting the Veterans Administration (VA) Mobility Screening and Solutions Tool
In the pursuit of optimizing the rehabilitation journey for our esteemed veterans, the Veterans Administration (VA) has developed the Mobility Screening and Solutions Tool. This tool aims to enhance early mobilization and improve the functional outcomes of veterans.

Early Mobility
Jun 27, 2023
5 Early Mobility Solutions to Optimize Veteran Recovery from In-Bed to Out-of-Bed Mobilization
The significance of early mobility in the rehabilitation of war veterans cannot be overstated. In fact, muscle wasting occurs early and rapidly during the first week of critical illness, with losses of up to 20% seen for those in multi organ failure1. By promoting movement at the earliest stages of recovery, we can unlock a multitude of clinical benefits and significantly improve the quality of life for our brave veterans.

Early Mobility
Jun 27, 2023
The benefits and barriers to Early Mobilization
Early mobilization has been demonstrated to be both safe and feasible for patients admitted to critical care.1
Safe patient handling
Jun 08, 2023
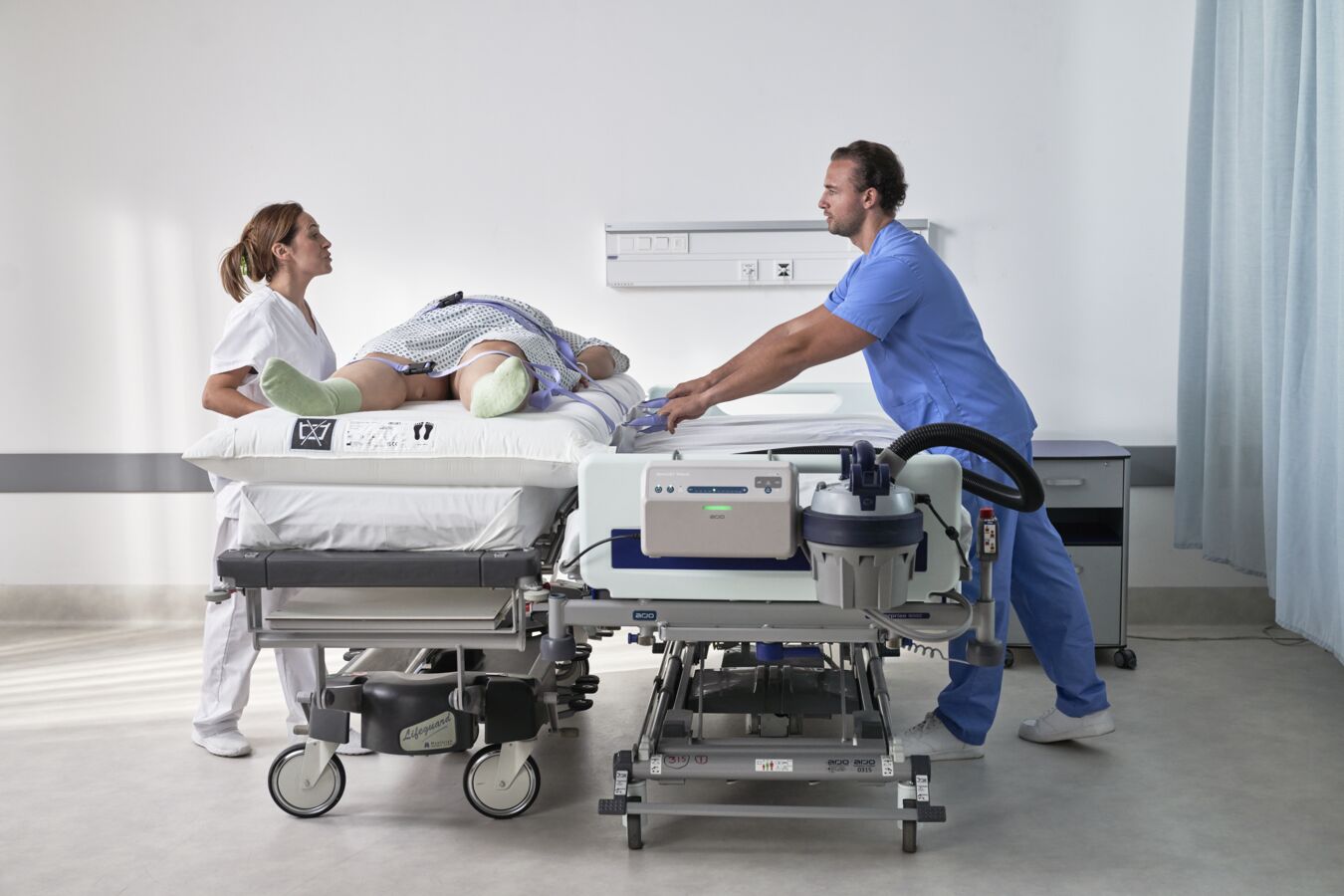
5 things to consider when choosing an air-assisted transfer device
The lifting and transferring of patients play a pivotal role in caregiver’s health and musculoskeletal injury risk, which can impact turnover and lead to staffing shortages, thus affecting overall levels of patient care¹,². This risk of injury has increased with the rising number of plus size patients seeking healthcare.³

Safe patient handling
Jun 08, 2023
AirPal: much more than a patient lateral transfer
With the AirPal® air-assisted patient transfer system, you can transfer patients from one surface to another and reposition within the bed safely, comfortably and efficiently. AirPal supports the patient on a bed of air, an elevating effect created by air flowing through the perforated underside of the AirPal transfer mattress, lifting the patient away from the bed surface.

Safe patient handling
Apr 11, 2023
Tips and techniques to consider when using slide sheets under the patient
Using slide sheet devices for in-bed movements has benefits not only for safety, but also for the patients’ comfort, security and dignity¹.
The risks of moving the full body weight of a dependent patient are well recognised. For horizontal transfers and many in-bed movements, the provision of a friction-reducing slide sheet may be a sound solution for reducing physical effort and improving patient comfort.¹,²

Safe patient handling
Apr 11, 2023
Do you consider these 7 factors in the patient mobility assessment process?
The International Standards for manual handling of people in the healthcare sector discuss various methods of assessment1. The most essential transfers take place multiple times throughout the daily journey. Risk assessment helps to identify the most appropriate transfer and equipment for the situation and activity to be carried out. This helps promote functional mobility and reduce the risk of caregiver injury.

Safe patient handling
Apr 11, 2023
5 solutions to support single-handed care
The term single-handed care simply refers to a means of safely transferring an individual with the correct equipment and appropriate number of carergivers.
In some care environments, there have long been ‘informal working practices’ automatically requiring the need for two caregivers when assisting with patient handling activities. However, in recent years there has been a definite shift towards the provision of single-handed care, especially within long-term care settings.¹

Safe patient handling
Apr 11, 2023
Preventing caregiver injuries: How floor and ceiling lifts can help
Routine care tasks should not put caregivers at risk. Caregivers perform transfer, repositioning and hygiene tasks many times throughout the day. If these essential care tasks are not performed with the right equipment, care processes and skills, they can put caregivers at risk of musculoskeletal disorders (MSD) and injury. It is recommended to use of the right mechanical assistive aids that can improve caregiver safety and reduce the high costs related to caregiver injury.¹
“Mechanical lifts reduce the back-compressive forces on nursing personnel by an estimated 60%”²

Safe patient handling
Apr 11, 2023
Key considerations for healthcare facilities planning
What is the space needed around the bed to make it easier to get in and out, to maneuver equipment, and for the caregiver to support residents when they need it with less risk of injury?
We understand that planning a facility around the needs of residents and to promote the ability of staff to care for them in a safe and effective way is imperative.
And the earlier it's done the more and better options you'll have and potentially lower overall costs significantly.

Safe patient handling
Apr 11, 2023
What’s the cost of caregiver injury and patient immobility in healthcare environments?
Patient handling injuries can be costly not only for the caregiver but also for the organisation. The financial impact is associated with injury investigation and potential claim management, temporarily replacing an injured caregiver and litigation/settlement costs. This article aims to evaluate the cost of caregiver injury and patient immobility in healthcare environments and identify potential solutions to mitigate these costs. Patient immobility can have a serious financial impact on the organisation and caregiver injury can result in fewer staff resources and reduced working efficiencies.
“The use of the right mechanical assistive aids improves caregiver safety and reduces injury related costs for the organisation”¹
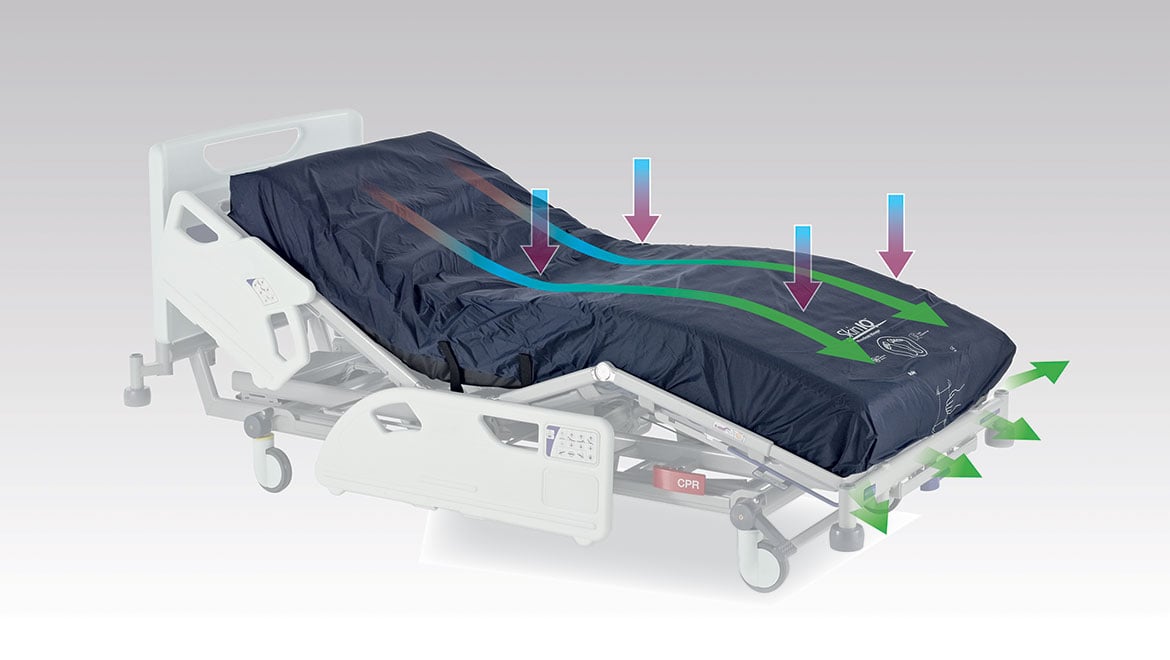
Pressure injury prevention
Apr 06, 2023
What’s Under the Sheets Does Matter
The National Pressure Injury Advisory Panel (NPIAP) recently held its annual conference in San Diego in March 2023. One of the posters submitted by our Arjo colleagues, “What's Under the Sheets Matters- a Compatibility Study,” was awarded the prestigious NPIAP 2023 Charlie Lachenbruch Award. This is the only award presented at the annual conference to industry partners for their contribution to the science of pressure injury (PI) prevention and treatment.
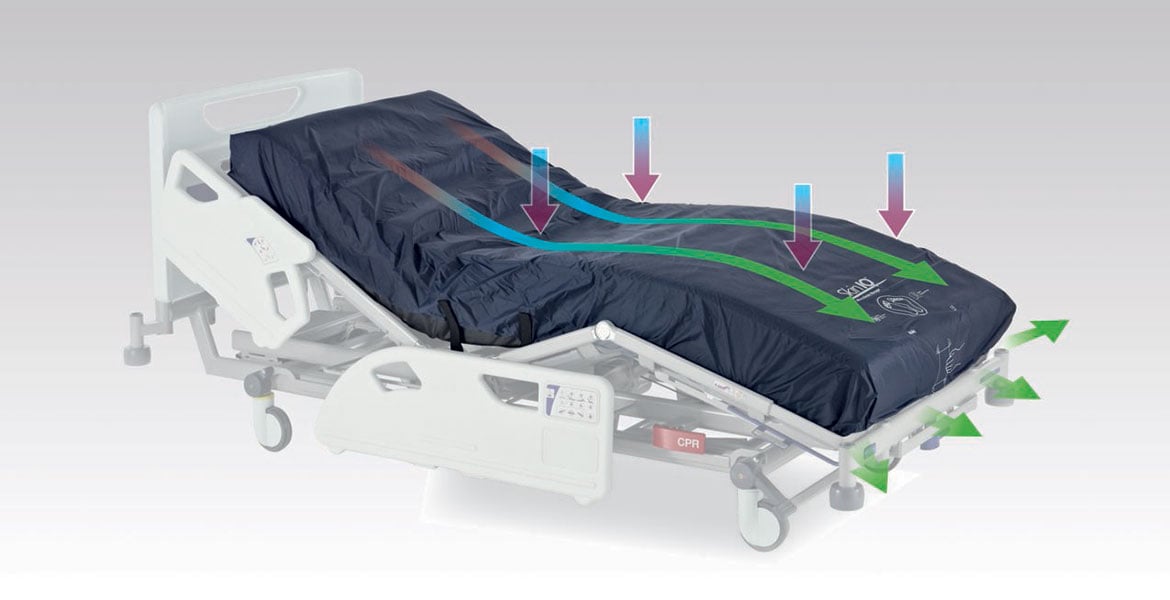
Pressure injury prevention
Mar 28, 2023
The time factor in alternating pressure
Why “Lower for Longer” is the driving principle behind the performance of an alternating pressure surface.

VTE prevention
Mar 08, 2023
Five key benefits of our upgraded VTE prevention solution Flowtron® Active Compression system
Providing a solution for the largest preventable cause of hospital deaths, venous thromboembolism (VTE) prevention is an important and growing area within Arjo. Our upgraded and improved solution, the Flowtron Active Compression System, is now launched – and here are the key benefits.

Mobility, Safe patient handling
Feb 15, 2023
Empowering movement: Mobility matters
Mobility is defined as the ability to move in one’s environment with ease and without restrictions.1
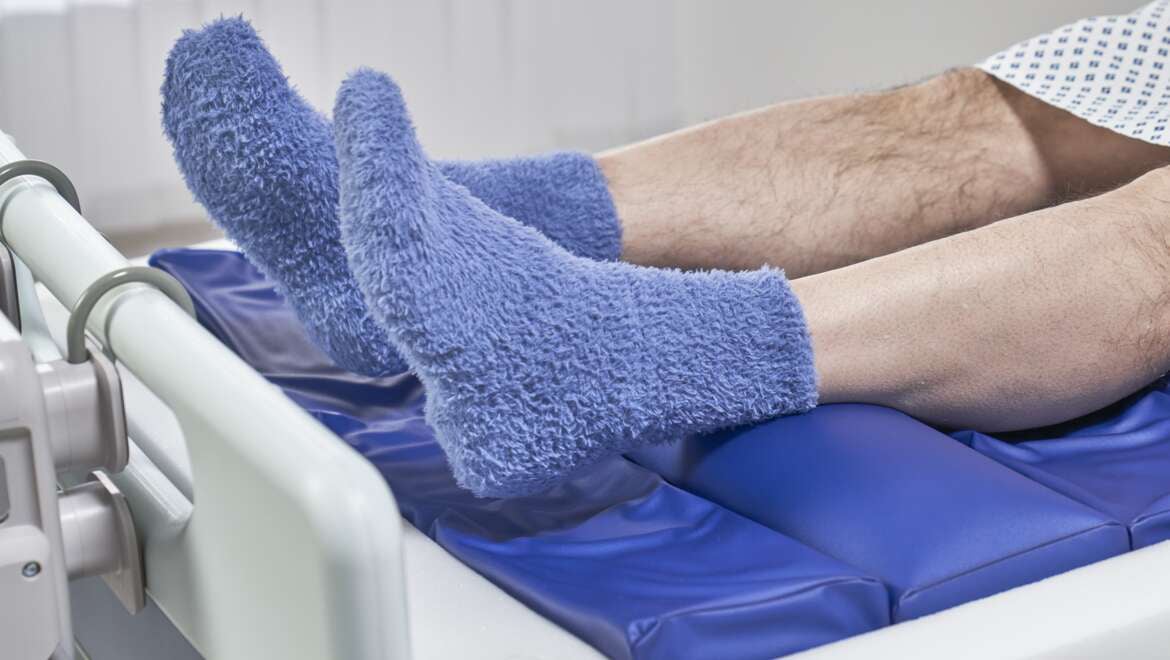
Bariatric
Feb 08, 2023
Bariatric care challenges and solutions
The Centers for Disease Control and Prevention notes that obesity is a national epidemic affecting more than one in three adults, causing higher medical costs and a lower quality of life.1,2

Pressure injury prevention
Dec 02, 2022
Preventing Pressure Injury in Prone Positioning
Prone positioning, which involves turning a patient over so that they lie in a chest-down, is a well-established intervention for ARDS. It has been shown to improve oxygenation and prevent ventilator-induced lung injury due to the more uniform distribution of lung stress and strain1,2.
_Blog%20Image_PNG.png)
Pressure injury prevention
Apr 24, 2022
How our cover fabrics are designed to support infection control
A mattress cover should support the prevention of cross-contamination – without compromising the performance of the support surface.
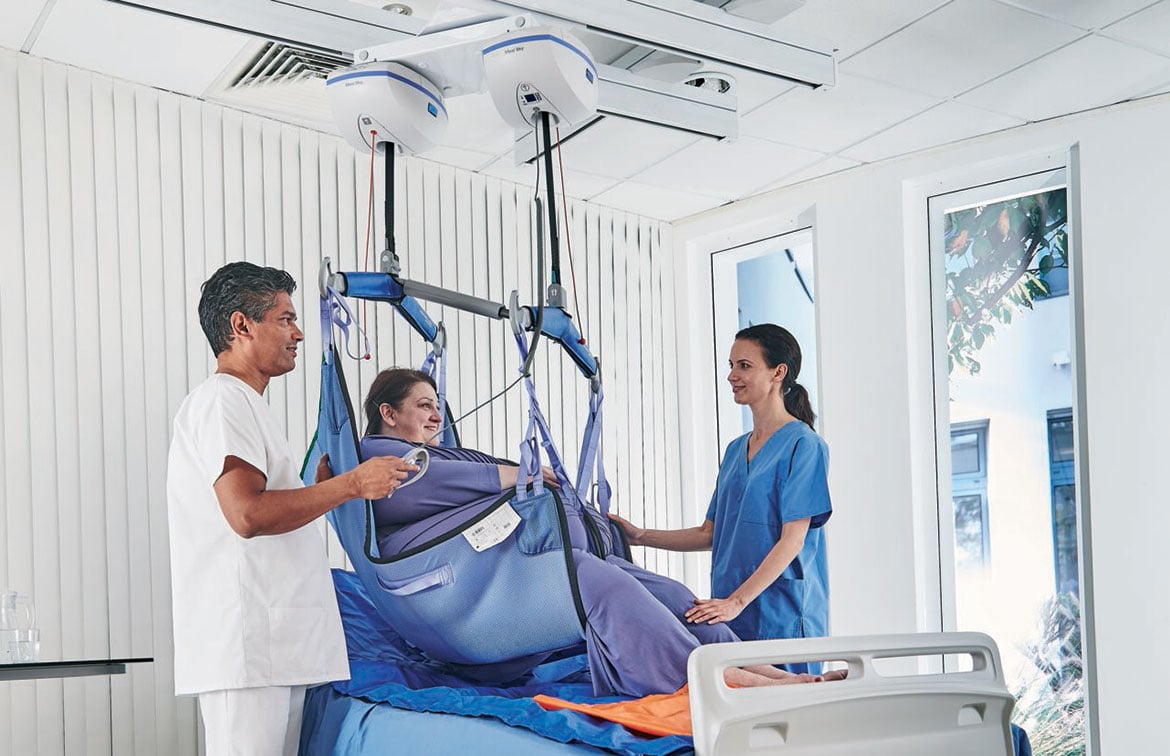
Microclimate management
Mar 15, 2022
Microclimate management: The critical link to skin integrity
As a clinician, have you ever had the experience of rolling a patient on to their side only to find their back is warm and sweaty without any indication of sweating elsewhere? Here is some insight into why this may have happened.
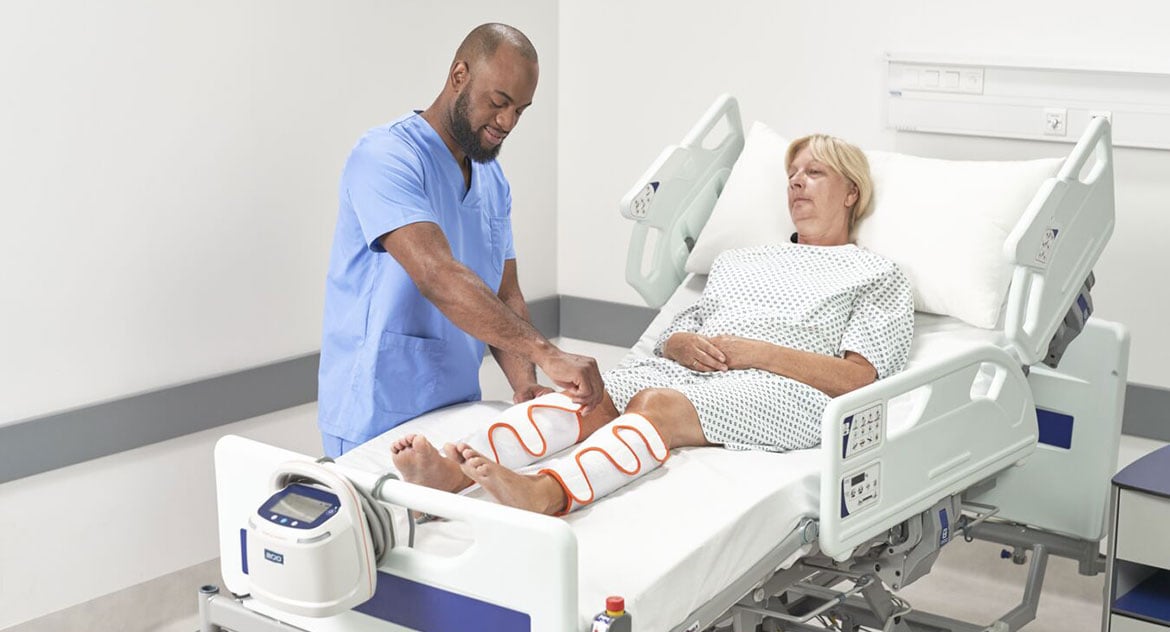
VTE prevention
Mar 03, 2022
DVT Awareness Month Webinar: Proven VTE Prevention Strategies
Arjo is committed to improving the everyday lives of people affected by reduced mobility and age-related health challenges. In honor of DVT Awareness Month (March), we support efforts to raise awareness of the potentially devastating impact of deep vein thrombosis (DVT) and pulmonary embolism, collectively known as venous thromboembolism (VTE).

Dementia
Jan 11, 2022
Meeting needs in dementia care
Alzheimer’s disease, the most common cause of dementia, is characterized by symptoms involving memory, language skills, thinking, and the ability to conduct simple daily tasks. It is a slowly progressive disease where brain neurons become damaged or destroyed.

Pressure injury prevention
Jan 04, 2022
The link between nutrition, pressure injuries and wound healing
Nutritional status plays an integral role in the process of wound healing and in the prevention and treatment of pressure injuries. Macronutrients and micronutrients are required by each organ system in specific amounts to promote growth, development, maintenance, and repair of body tissues.1
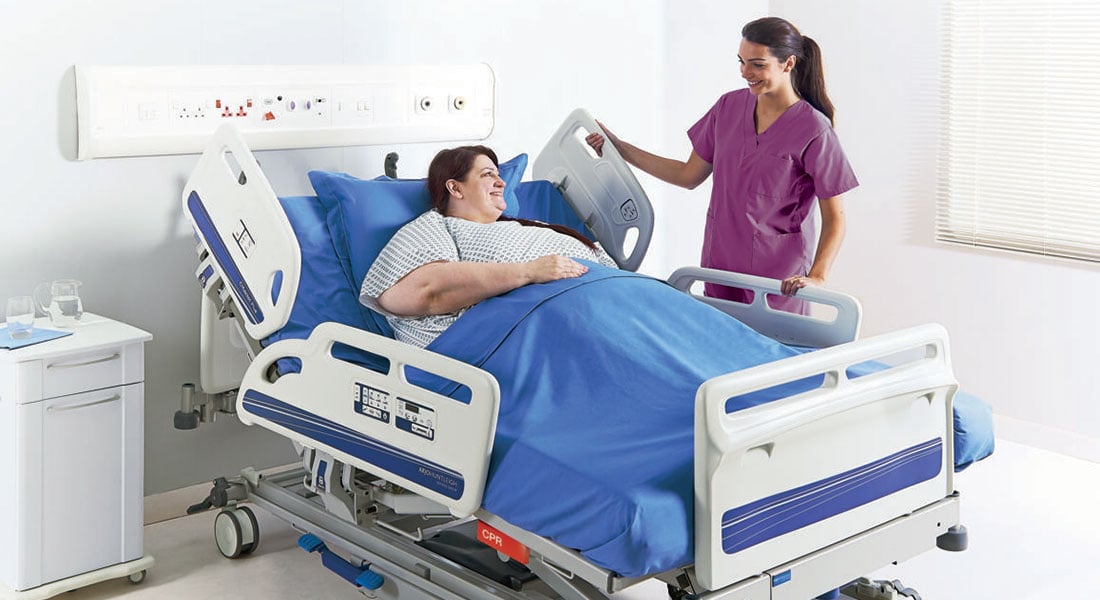
Bariatric
Dec 15, 2021
A clinician's perspective: Bariatric medical beds for a safe & dignified care environment
According to recent data (2020) from Trust for America’s Health, the US adult obesity rate of 42.4% continues to grow over the years and is the first time the national rate has passed the 40% threshold.1
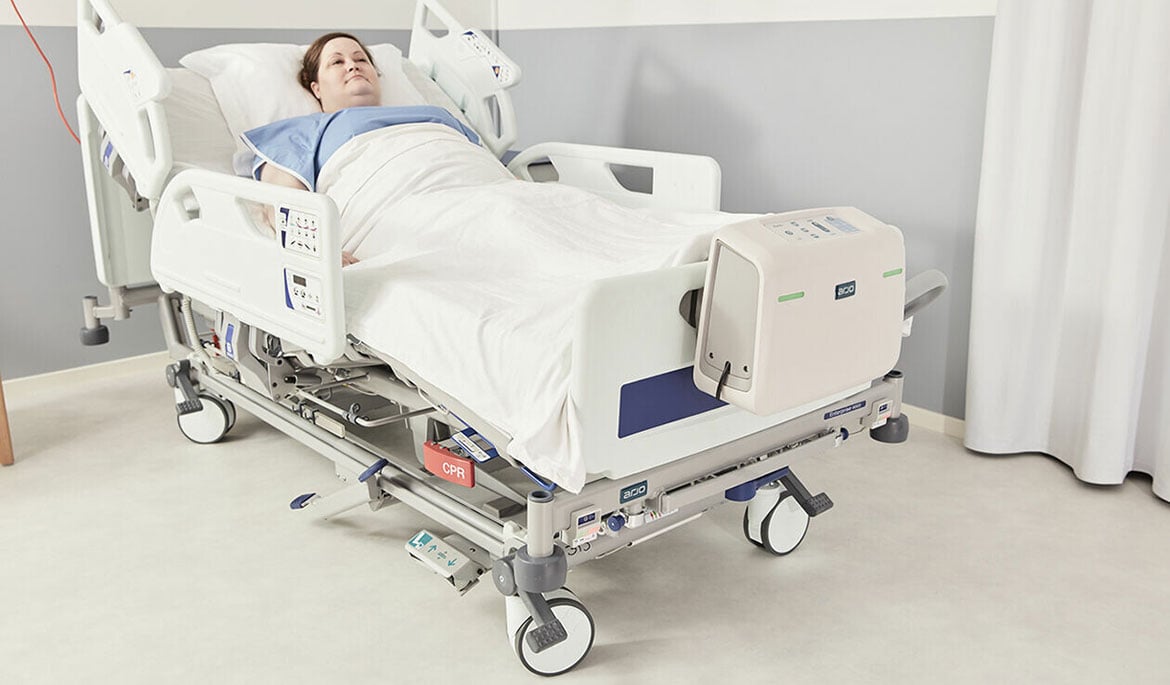
Pressure injury prevention
Dec 10, 2021
Pressure injury prevention strategies for healthier outcomes
A pressure injury seriously affects quality of life. As clinicians, increasing awareness of pressure injury prevention and education are important to help ensure healthier outcomes for those in our lives and under our care.

Clinical insights
Dec 02, 2021
Clinical Insights: Person-centered dementia care with the Wellness Nordic Relax Chair
We recently spent time with Mary Anne Uayan, BSN, RN, CCRN, CWCA, Arjo Clinical Consultant - Wound Care, to discuss the advantages of the Wellness Nordic Relax Chair. Mary Anne has been a nurse for over 23 years, is certified in adult critical care and wound care, and has extensive experience as a wound care champion during those years. She initially joined Arjo’s Critical Care team as a Clinical Consultant for critical care therapies and now is an integral part of the Wound Care team.
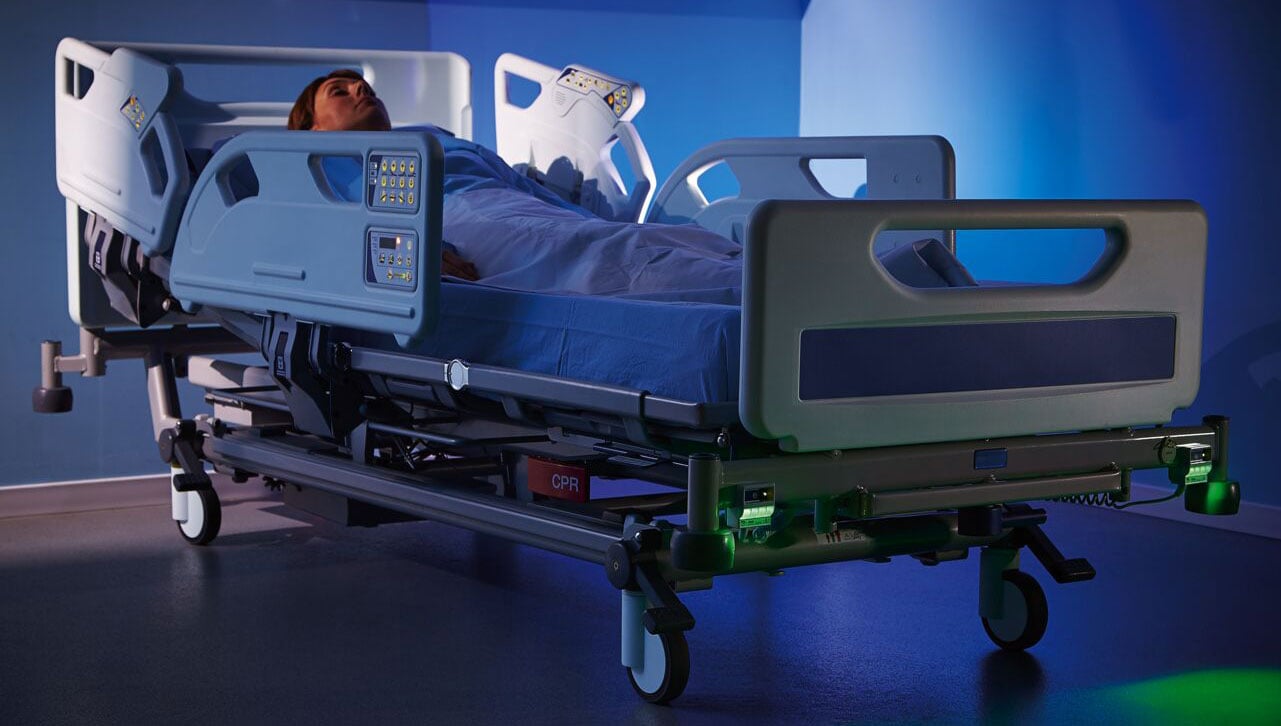
Clinical insights
Nov 18, 2021
Clinical Insights: Medical beds, fall prevention and a safer care environment
Today, we welcome Bob Andersen, RN, WCC, Arjo Clinical Consultant, to discuss medical beds and fall prevention. Bob has served in the Navy and has worked in CVICU, ER, Trauma, Neuro Interventional, Burn/Hyperbaric ICU, and more recently worked as a Flight Nurse. He has a passion for wound care and patient safety, and works closely with hospital staff and educators to help establish a safe environment for both healthcare staff and patients.
Safe patient handling
Nov 12, 2021
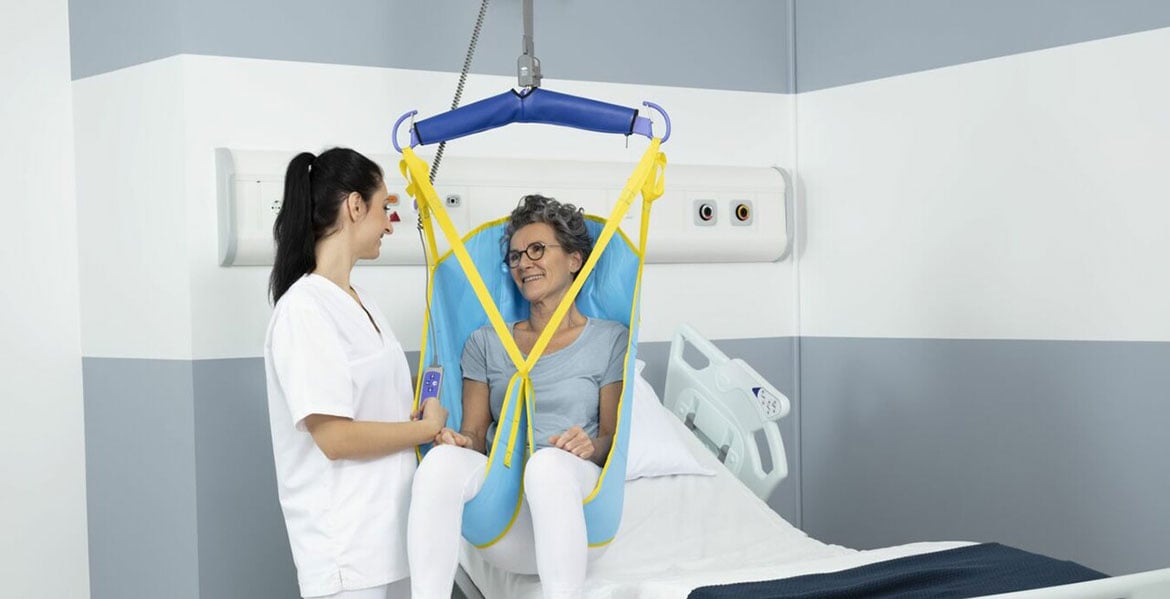
Ceiling lifts – A safe patient handling solution
Ceiling lifts provide a multitude of benefits to the healthcare facility as a safe patient handling solution. Take a look at several examples below that are supported by clinical documentation.
Safe patient handling
Nov 04, 2021
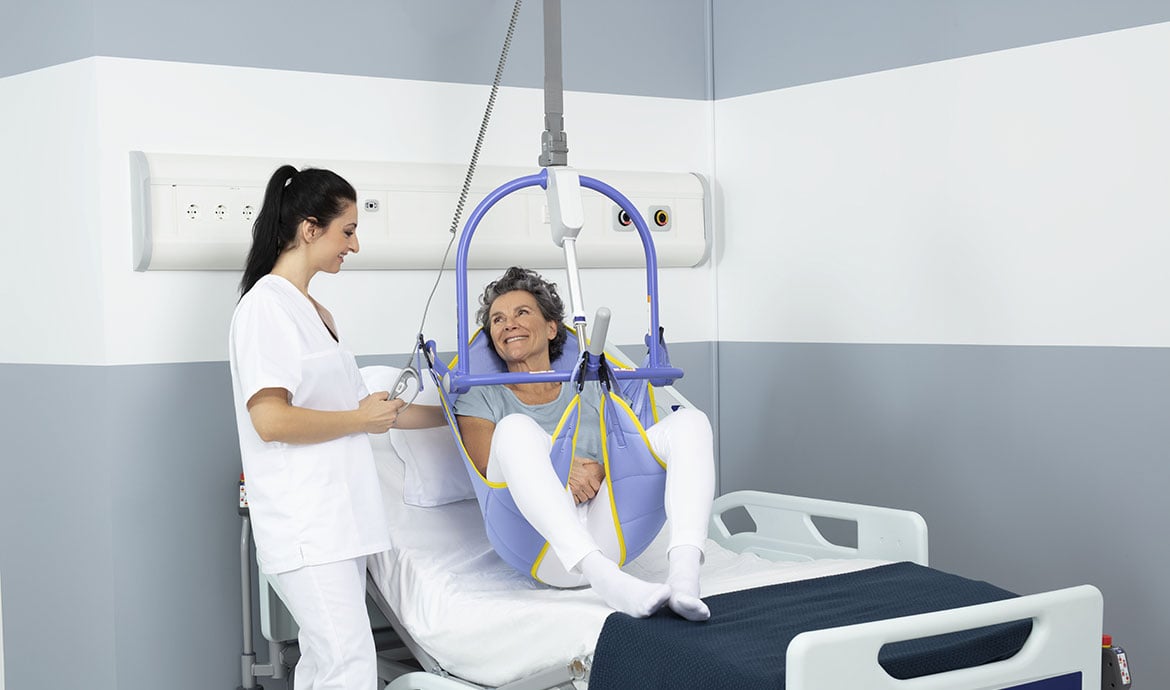
Ten advantages of ceiling lifts in a healthcare environment
In healthcare, architects and owners collaborate to keep staff and patients safe as well as plan for the best use of space in a facility. Ceiling lifts provide a high level of satisfaction to those who incorporate this technology into their project plans. Below are 10 advantages of ceiling lifts in a healthcare project.

General
Nov 02, 2021
November is Long-Term Care Awareness Month
For the past 20 years, November has been recognized as National Long-Term Care Awareness Month. By 2030, one in five residents in the US will be age 65 or older, and the number of those in need of long term support services in the US is already at 14 million and expected to grow to 27 million by 2050.1
General
Oct 13, 2021
World Thrombosis Day: Our eyes are open to thrombosis
In recognition of World Thrombosis Day on October 13th, Arjo embraces efforts to raise awareness of thrombosis with our “eyes open to thrombosis” on this day and every day. World Thrombosis Day is the birth date of Rudolf Virchow, a German physician and pioneer, who studied the etiology and pathophysiology of thrombosis, and advanced our understanding of thrombotic conditions to this day.
Clinical insights
Oct 06, 2021
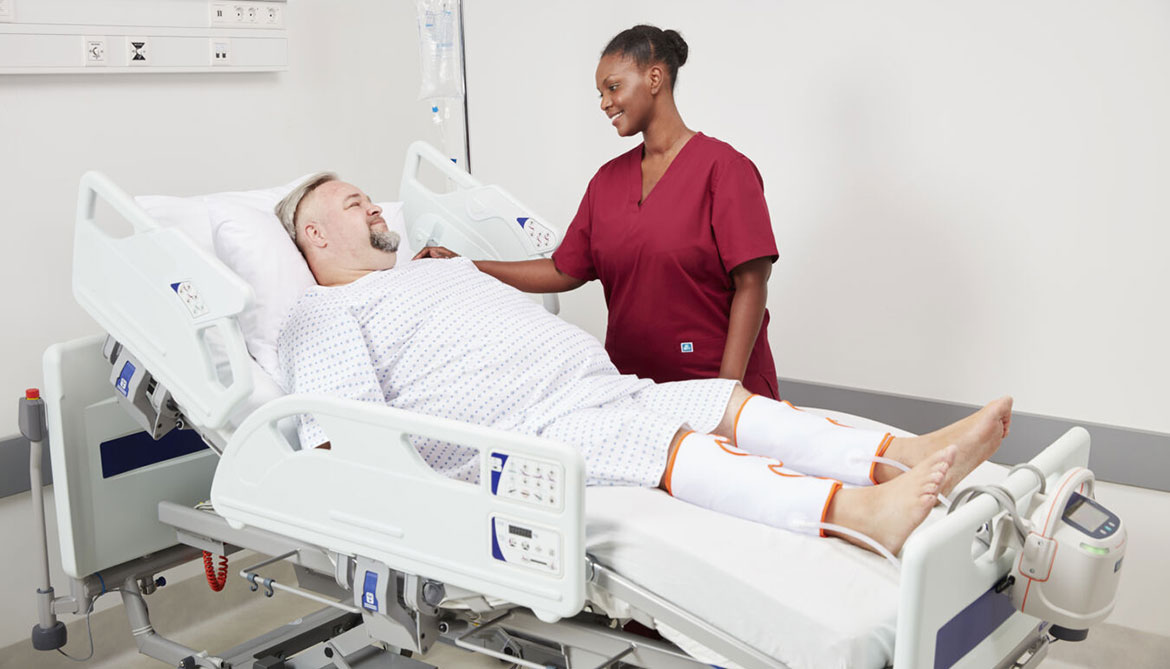
Clinical Insights: Voice of customer for the Flowtron ACS900 pump & Tri Pulse sequential garments
Today, we welcome Grace Hukushi, RN, BSN, Arjo Clinical Manager, to discuss voice of customer research conducted with clinical end-users of the Flowtron ACS900 pump and Tri Pulse sequential garment range in several countries.

General
Sep 01, 2021
September is World Alzheimer’s Month
For the past decade, September has been designated as World Alzheimer’s Month to raise awareness internationally of this devastating disease, with World Alzheimer's Day celebrated annually on September 21.
Clinical insights
Aug 06, 2021
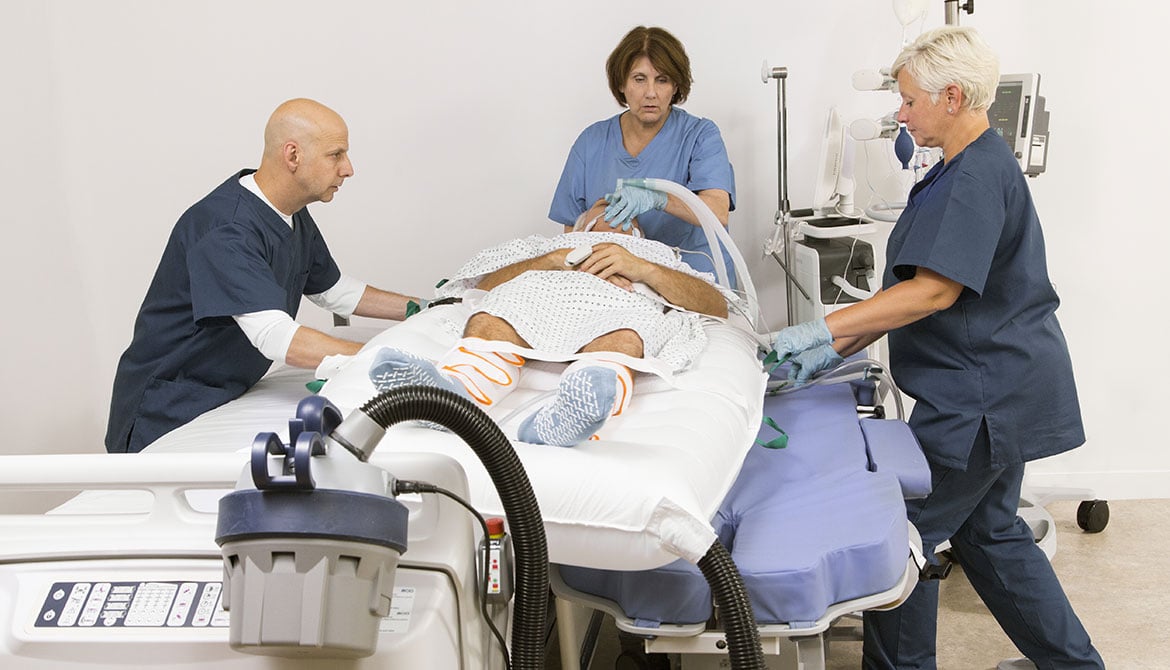
Clinical Insights: Reduce injury risk and promote safety with the AirPal system
Today, we welcome Ali Qureshi, OTR, MOT, Arjo Clinical Consultant and Occupational Therapist, to discuss Arjo’s newest safe patient handling and mobility aid, the AirPal® lateral transfer and repositioning system.
Pressure injury prevention
Aug 05, 2021
Wound care requires an individualized approach
Recovery from a wound, whether a stage 1 pressure injury or a full thickness wound, requires an individualized approach. The acronym, APIE, frequently includes trial and error, and complex testing to the find the right solutions at the right time to heal a wound:
A - Assessment
P - Planning
I – Intervention
E - Evaluation

General
Jul 21, 2021
Investing in our future
Our environment is fragile and the focus this year is to “restore our earth” through natural processes, green technologies and innovation.
Safe patient handling
Jun 16, 2021
Rehabilitation: Occupational therapy and patient handling perfectly aligned
With a holistic focus on mind and body, occupational therapy and safe patient handling (SPH) complement each other because of the importance that mobility plays on improving one’s overall quality of life.

Pressure injury prevention
Jun 06, 2021
How to prevent pressure injury during patient rehabilitation
Empowering movement is fundamental to any patient rehabilitation programme and is a core principle in the prevention of pressure injury development. With the impact of the current pandemic, the focus on mobilising and rehabilitating patients earlier and often throughout the day has never been higher.

Pressure injury prevention
Jun 03, 2021
Meeting the infection control challenge when selecting a support surface
Healthcare settings face the challenge of managing an effective Infection Control protocol on a daily basis. Ensuring the safety of patients and staff at all times, in a range of different settings requires a robust process, where care and treatment can be delivered without the risk of infection due to poor hygiene standards.

Dementia
Jun 03, 2021
Raising Awareness of Alzheimer’s & Brain Awareness Month
As you read this blog, someone in the world will develop dementia every three seconds! In observance of this public health priority, the month of June has been designated by the Alzheimer’s Association as a time to “go purple or wear purple” in support of raising awareness of Alzheimer’s disease and to recognize caregivers for their support of those in their care.

Pressure injury prevention
Jun 02, 2021
Preventing Pressure Injuries in Patients with Reduced Mobility
Reduced mobility is a significant risk factor for pressure injury development, international guidelines emphasise the need for regular turning and repositioning of patients to help prevent skin damage¹. While a pressure redistribution mattress may enable the repositioning regimen to be individualised, regular postural change is still important but not without risk to the patient or caregiver.

Pressure injury prevention
May 31, 2021
How to manage microclimate in the plus sized patient?
According to a 2016 report by the WHO, globally there are 650 million people that are obese accounting for approx. 13% of the world’s adult population¹.

Mobility
May 26, 2021
Mobility is life: Empowering movement
Mobility is life. When people move, they are able to engage with their environment. Playing ball with a child, cooking a meal with friends or simply walking down the street… all these types of activities help to create meaning in our lives. Unfortunately, life can be unexpected and changes due to illness or injury can impair our ability to fully engage.

General
May 07, 2021
Celebrating You this National Nurses Week & Month
National Nurses Week begins each year on May 6 and runs through May 12, Florence Nightingale’s birthday. Florence Nightingale, a revolutionary figure in nursing, is known as the “lady with the lamp,” with the lamp representing nursing’s selfless work and dedication. Nursing is a science and an art that focuses on promoting the quality of life as defined by populations, communities, families, and individuals throughout their life experiences from birth through the end of life.

Hygiene
May 05, 2021
It’s in our hands!
Since 2009, observing World Hand Hygiene Day on May 5th each year is an opportunity for us to stop and reflect on how important hand cleanliness is, not only for ourselves, but how our attention to this action can affect the rest of the world. This year’s campaign theme to promote global awareness is “achieving hand hygiene at the point of care” as “seconds save lives – clean your hands.”1

Pressure injury prevention
May 03, 2021
Empowering movement to prevent pressure injury during patient rehabilitation
Empowering movement is fundamental to any patient rehabilitation program and is a core principle in the prevention of pressure injury development. With the impact of the current pandemic, the focus on mobilizing and rehabilitating patients earlier and often, throughout the day, has never been higher.
Pressure injury prevention
Apr 07, 2021
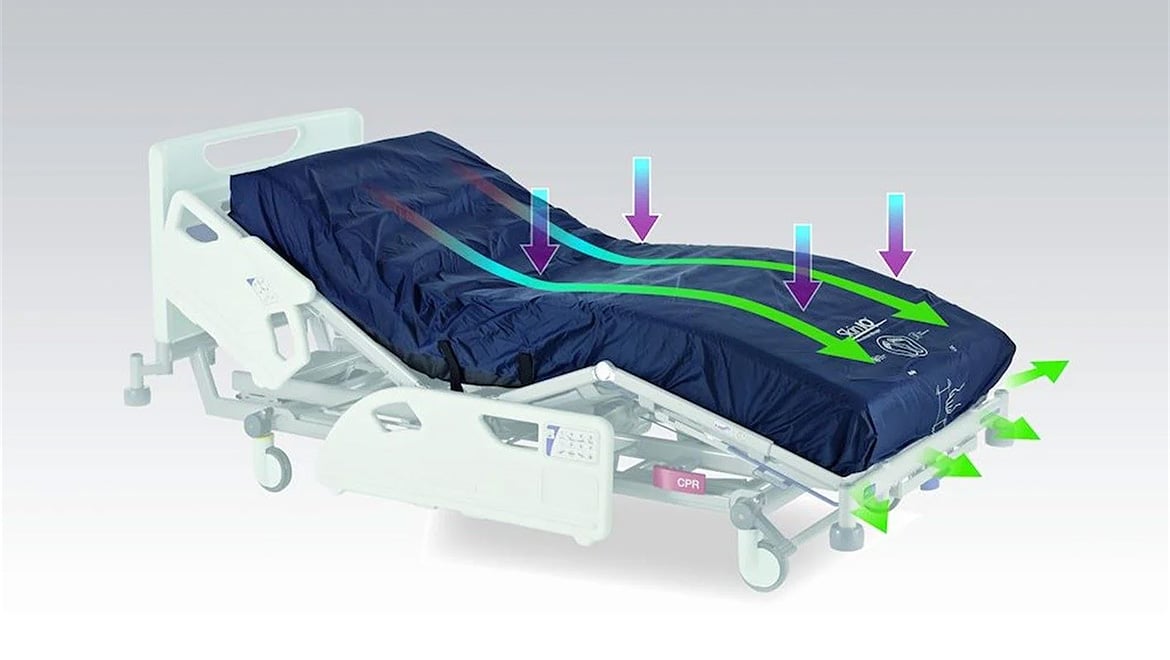
Managing skin microclimate with Skin IQ's Negative Airflow Technology
The International Pressure Ulcer Prevention and Management Guidelines discuss how managing microclimate can provide an environment conducive to injury prevention and tissue repair. As such the guidelines recommend the need for additional features such as the ability to control moisture and temperature when selecting a support surface.