Moving for recovery
By placing a focus on mobility early and regularly in a patient’s recovery pathway, the opportunity for rehabilitation is optimised. Our new Rehab Guide - "Rehabilitation through Empowering Movement" offers suggestions to assist and enhance moments for mobility by introducing technology as a supporting aid in rehabilitation therapy.
We aim to help caregivers recognise opportunities for patient mobility around the clock, and to support therapists and caregivers with innovative ways of using equipment for clinically validated rehabilitation and mobility activities.

”Helping ICU patients to be awake, mobile, and aware of their surroundings without fear has never been more challenging or important. Consistent early mobility is an essential part of restoring people beyond survival and toward recovery, back at home.”
Heidi Engel, Critical Care Clinical Specialist
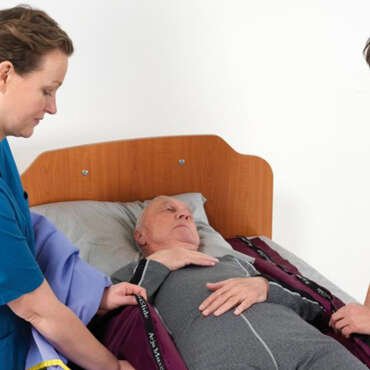
Sitting a patient on the edge of the bed forms an important part of the early patient assessment, structured rehabilitation and seating plan.
Sitting on the edge of bed provides neurological stimulus to aid waking and orientation.¹
Activities may include:
- Sitting on the edge of the bed with multiple caregivers
- Core movements on the edge of the bed using a slide sheet
- Sitting on the edge of the bed with a passive lift and sling
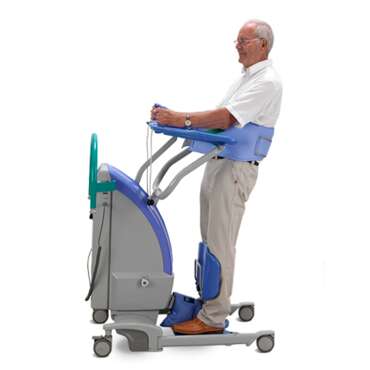
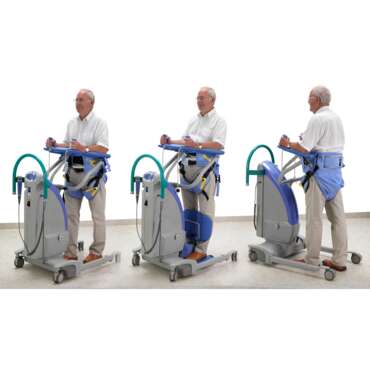
- Sitting on the edge of the bed with an active lift
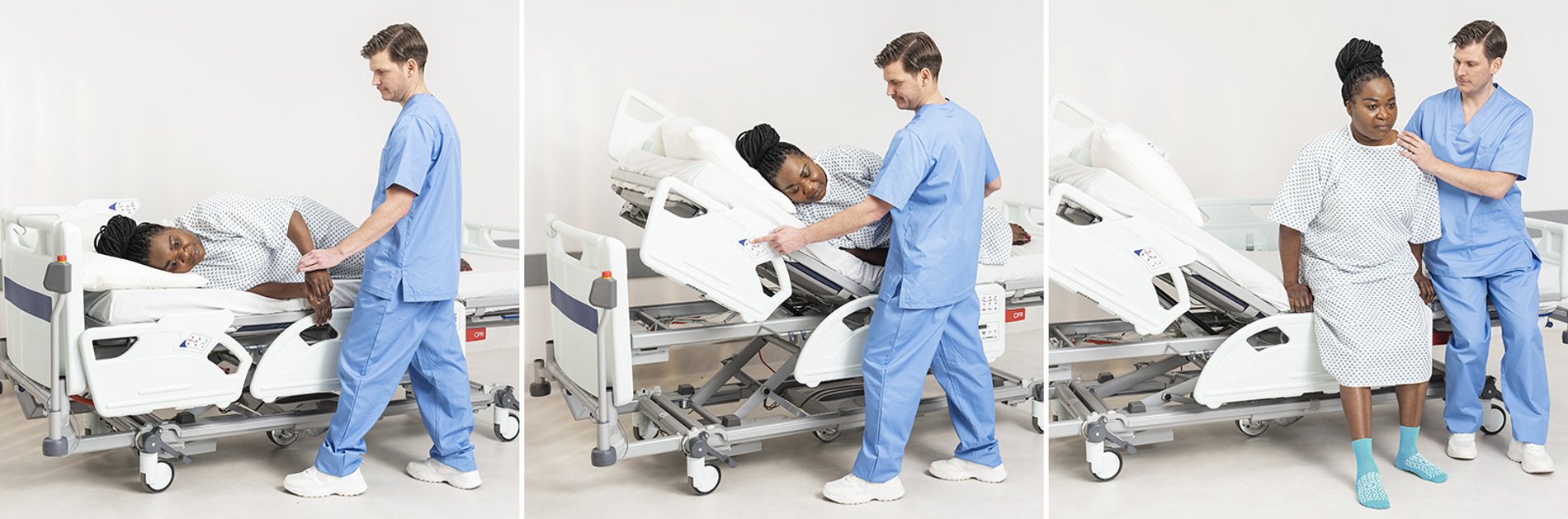
”We would not be able to get the majority of our patients to engage in early rehab without the correct tools” James Bruce, Occupational Therapist
A person’s body shape and size, the supporting surface, and even their health or emotional state can influence their seated posture.
Effective seating can help to:²
- Reduce muscle atrophy
- Improve sitting balance, strength and conditioning
- Increase environmental awareness
- Improve quality of life, well-being and participation in functional rehabilitation activities

”Rehab is a continuum. Appropriate equipment allows patients to progress while maintaining the safety of them and their caregivers.” Dr David McWilliams, Consultant Physiotherapist
Facilitate increased proprioceptive feedback through the load bearing joints
- The orthostatic challenge provided by this early verticalisation can help to reduce the deterioration in vital body systems or act as an early challenge for those with postural hypotension
- Prevent or reduce the impact of bone demineralisation³
- Recruit muscle activation considering autonomic response of vital body systems
- Environmental orientation to provide a better position for communication, eating and drinking or functional activities
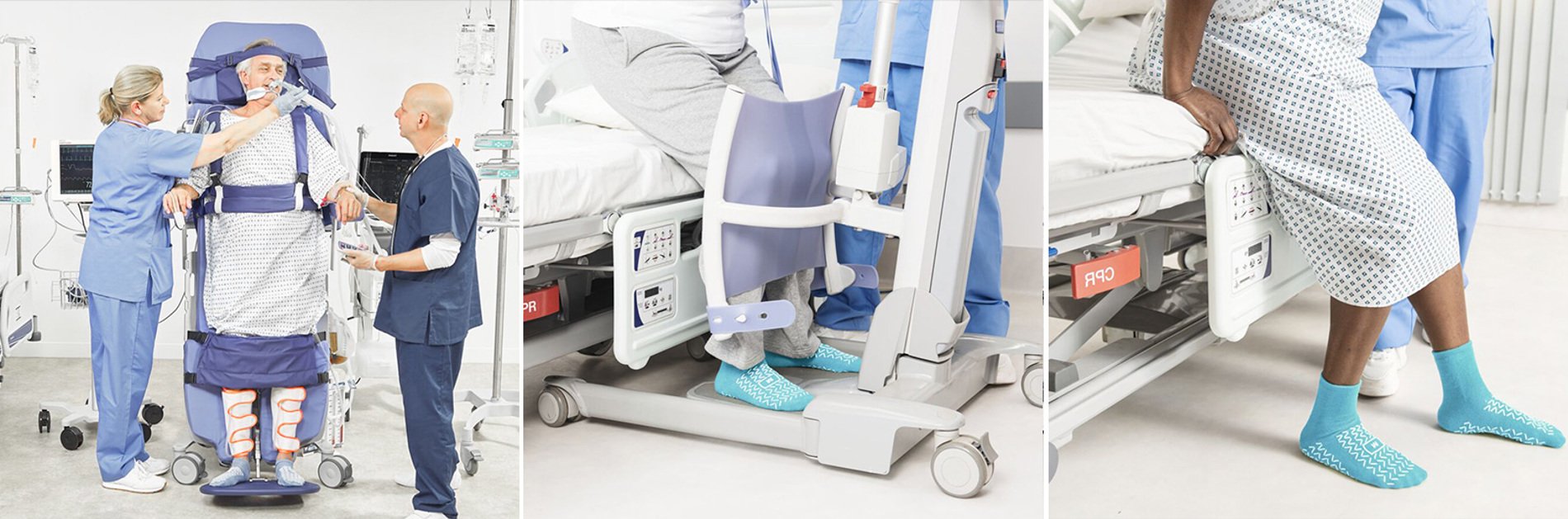
”Confidence that both the patient and caregiver are safe during an exercise session, freeing up hands to facilitate movement patterning.” Tracy Fulcher, Neuro Physio
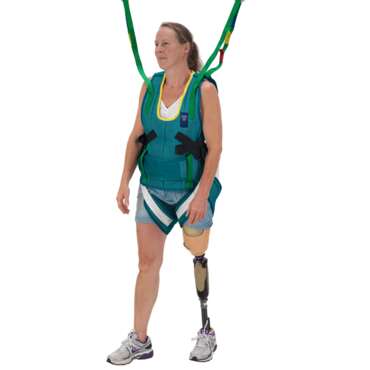
Rehabilitation programmes recognise the importance of focusing on the individuals specific activities of living that are meaningful to them. Technology can help to provide additional support to practice some of the activities that the patient would normally do at home such as:
- Cleaning and domestic activities
- Playing sport or engaging in activities with children
- Dancing
- Negotiating obstacles in everyday life
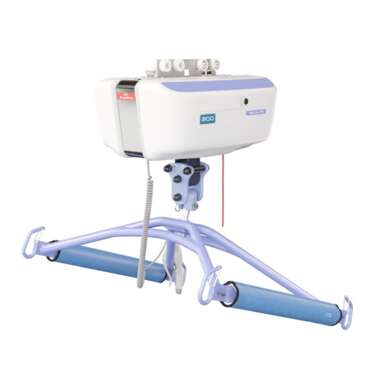
Using a ceiling lift with an ambulation sling can give the all important support to the patient, allowing the therapist to facilitate these meaningful and realistic activities.
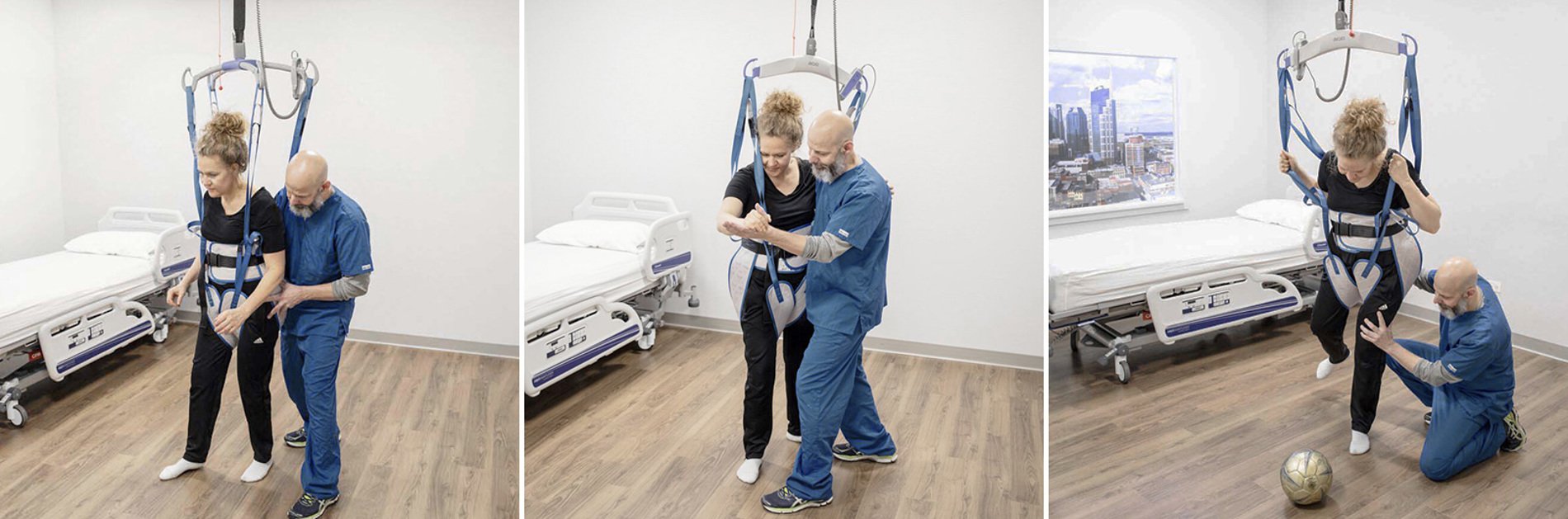
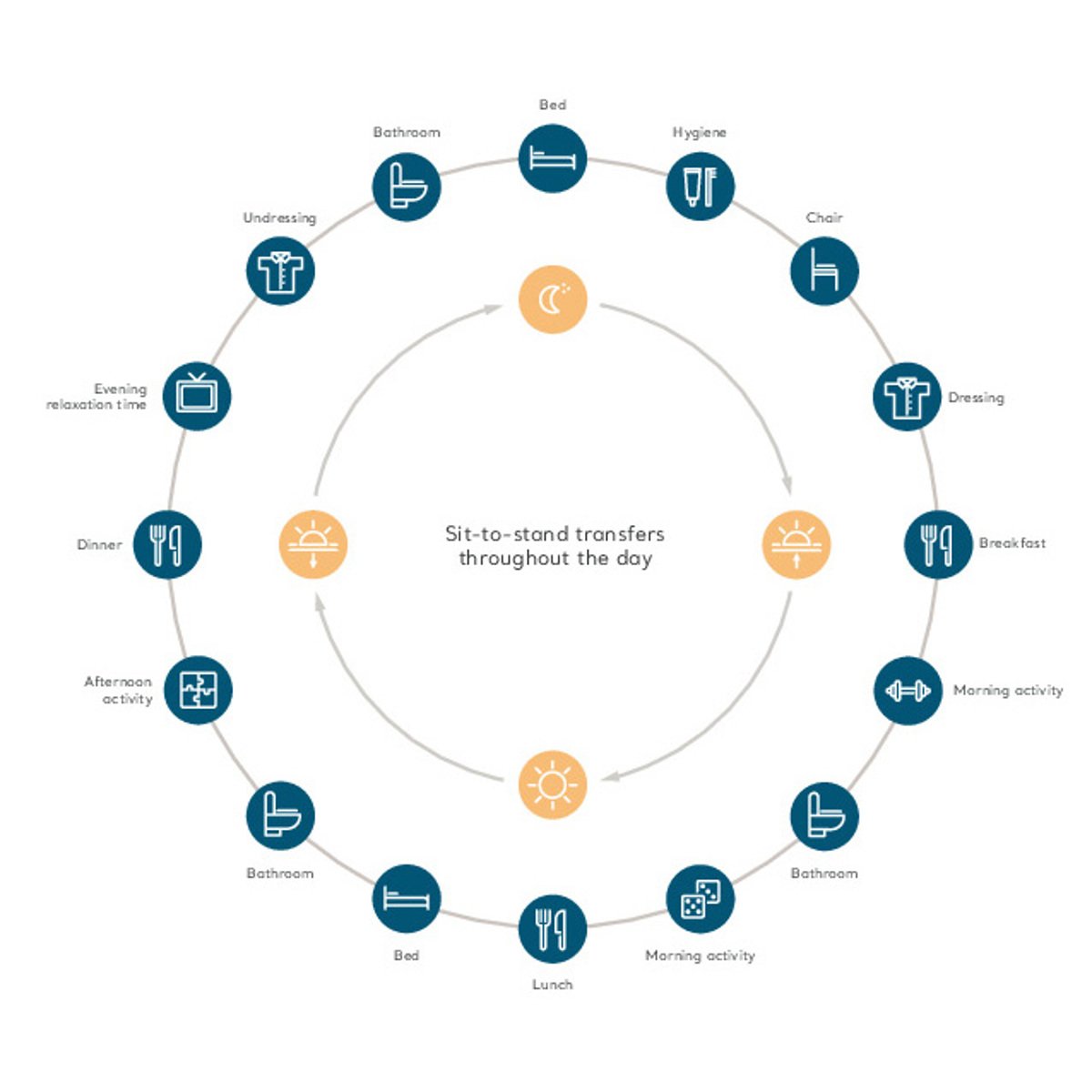
Maximising opportunities to empower mobility: Mobility moments through the day
A clinical study to monitor mobility levels early during a hospital stay, identified that on average, older hospitalised patients spent 83% of their time lying in bed, despite the ability to walk independently.⁷
Caregivers need to consider how often their patient has moved each day. Have they utilised all opportunities to encourage and support mobility whenever possible?
References
- Chang AT, Boots RJ, Brown MG, et al. Ventilatory changes following head-up tilt and standing in healthy subjects. Eur J Appl Physiol. 2005;95(5–6):409– 17 Cited in Clinical Evidence Summary – ICU Early Mobility Solutions published by Arjo. A00007.1.2.UKI.EN in March 2020
- Carr J.H., Shepherd R. B., (2011) Neurological Rehabilitation, Optimising motor performance. Second edition, Churchill Livingstone, Published 27th July 2010 Paperback ISBN: 9780702040511, eBook ISBN: 9780702044472
- Burnfield J, McCrory B, Shu Y et al (2013). Comparative kinematic and electromyographic assessment of clinician and device assisted sit-to-stand transfers in patients with stroke. Physical Therapy, 93(10): 1331-1341
- Guidelines for Care: Person-centred care of people with dementia living in care homes 2011 https://alzheimer.ca/en/Home/We-can-help/Resources/For-health-care-professionals/culture-change-towards-person-centredcare/guidelines-for-care Accessed 15-10-2020
- https://www.england.nhs.uk/wp-content/uploads/2016/04/ rehabilitationcomms-guid-16-17.pdf Accessed 25-9-2020
- NHS (2014). Rehabilitation, reablement and recovery. Rehabilitation is everyone’s business: Principles and expectations for good adult rehabilitation. Wessex Strategic Clinical Networks. Retrieved from: https://www.networks.nhs.uk/nhs-networks/clinical-commissioning-community/ improving-adultrehabilitation-services/principles-expectations
-
Brown, C.J., Redden, D.T., Flood, K.L. and Allman, R.M. (2009), The Underrecognized Epidemic of Low Mobility During Hospitalization of Older Adults. Journal of the American Geriatrics Society, 57: 1660 1665. https://doi.org/10.1111/j.1532-5415.2009.02393.x