Including VTE prevention solutions in surgical procedures to positively impact patients’ health and wellbeing
While healthcare facilities are aware of the risk of venous thromboembolism (VTE), care providers do not always have the time, training or resources to implement optimal prevention strategies. Learn how a clinic in Scandinavia has succeeded in integrating VTE prevention solutions in their surgery routines to safeguard the wellbeing of patients.
VTE is a serious condition that causes death and disability worldwide, with 10 million cases diagnosed each year1. Put simply, blood clots do not discriminate – the condition can affect people from all walks of life regardless of age, ethnicity, or gender2, in particular those who undergo surgery3.
Akademikliniken in Stockholm, Sweden, is one of Scandinavia’s leading cosmetic surgery clinics. For the past ten years, they have been using mechanical prophylaxis in the form of intermittent pneumatic compression (IPC) as a standard part of their routines for any longer surgery. Initially there were concerns from the staff that this was an extra step in the process that would only result in less time to complete each operation. Now, having seen and understood the positive effects, no one at the clinic questions it.
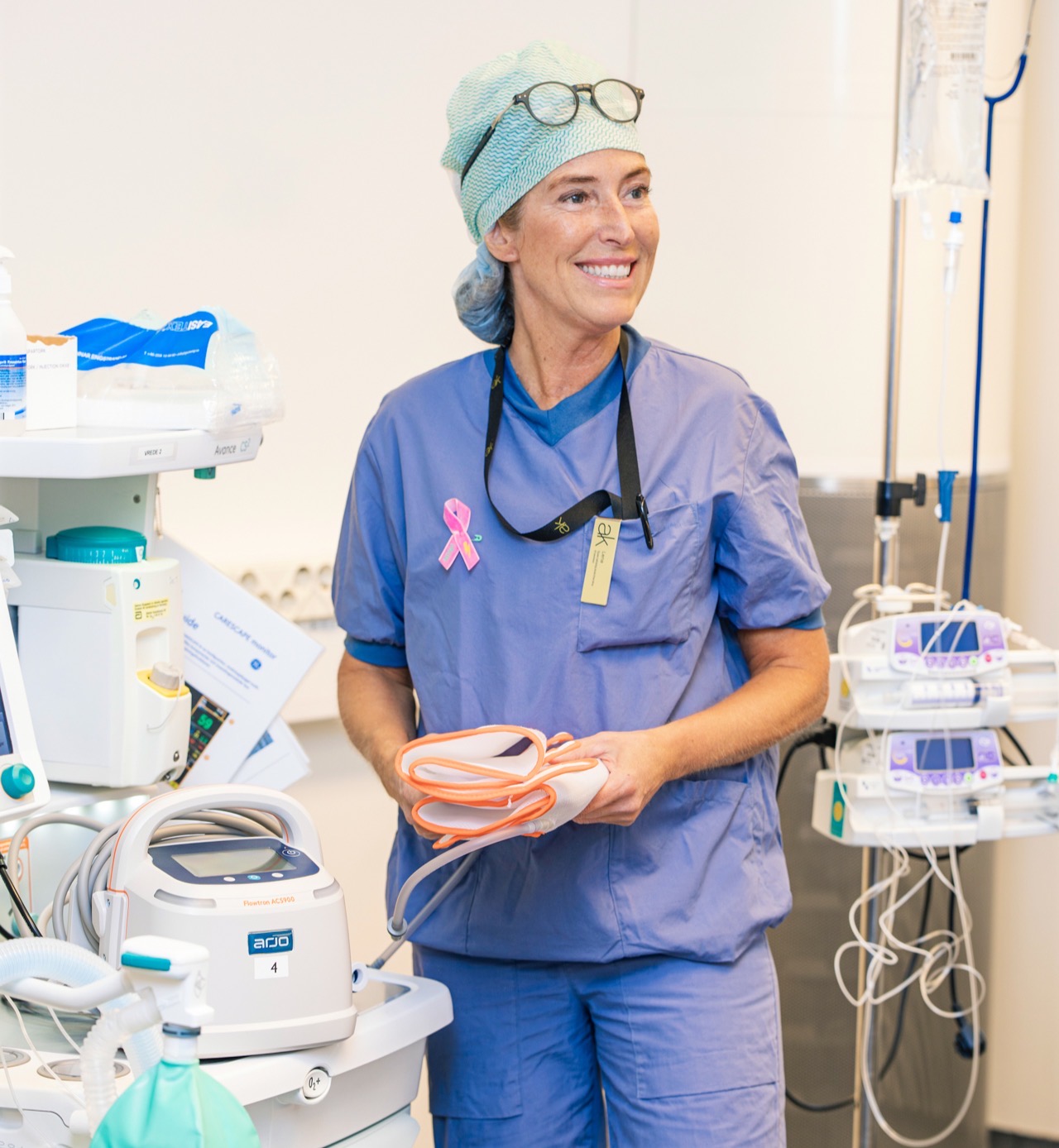
Preventive work is about changing mindset and culture
Lena Erkesjö, anesthesia nurse at Akademikliniken, explains how important it is to instil trust in each patient. Usually there is a lot of nervousness involved prior to an intervention, and every surgery has been preceded by an extensive dialogue that can span months.
“We talk patients through what each step in the process means, which is why there are no questions asked once we get to the part of placing the garment on the patient’s leg before surgery – and why it stays on afterwards,” Lena says.
“The routines for this are like clockwork, but it has taken education, determination and a cultural change in how preventive measures are viewed. Without the insistence from our head anaesthetist, we would not be where we are today with this type of preventive work,” Lena Erkesjö concludes.
Reducing the risk of one of the most common post-surgery complications
Patients undergoing surgical procedures lasting more than 60 minutes are considered one of the most significant risk groups for developing VTE, and the risk remains high several weeks post-surgery.
“To reduce the risk of bleeding during surgery, we want to avoid using blood thinning medication. However, we saw that when we removed that type of medicine, the occurrence of blood clots increased and that’s when I started to look into how we could work to prevent that kind of development through non-pharmacological solutions,” says Thore Hedestig, Physician specialist in anaesthesiology and intensive care, and continues:
“Using an IPC solution really makes a significant impact in terms of providing our patients with the best and most pleasant experience possible – significantly reducing the risk of one of the most common post-surgery complications. Actually, you could say that with this preventive approach, adding IPC as the VTE prevention method is physically similar to being out for a nice long walk – while anesthetized.”
He explains that during the Covid-19 pandemic, there was an increased focus on blood clots in general – but at the same time, resources for preventive work declined due to the extra strain put on all healthcare.
“Our patients are usually healthy; otherwise we wouldn’t go through with surgery. Even if the patients are not considered high risk of developing VTE, we definitely see that VTE prevention solutions have a positive impact on our patients’ health and wellbeing – which ultimately also reduces costs and the demand on resources for the healthcare system as a whole. We are lucky to have management supporting these types of investments in prevention. Imagine the positive impact we could see if VTE prevention protocols including IPC were used more widely in healthcare,” says Thore Hedestig.
Focusing on the long-term positives
According to Martina Kroon, who is a trained nurse and works as a Product Specialist with Arjo Sweden, it is unusual for a private cosmetic surgery clinic to invest in mechanical prophylaxis, and she finds it inspiring that Akademikliniken really has integrated the preventive approach into their way of working.
“While others may see this solution as an added cost, the team at this clinic has truly seen the positive effects in fewer post-surgery issues, like deep vein thrombosis and pulmonary embolism. In my view, this should be the benchmark for high quality surgery. If all healthcare providers were empowered to always prioritise the long term positives over the short term costs – patients would experience fewer complications and have increased quality of life, while providers would optimise costs and efficiencies in care, leading to more sustainable healthcare systems.”
Learn more about VTE prevention solutions here
Download our clinical evidence brochure on VTE here
References:
1 Jha AK, Larizgoitia I, Audera-Lopez C et al. The global burden of unsafe medical care: analytic modelling of observational studies. BMJ Qual Saf 2013; 22: 809-15.
2 Geerts WH, Pineo GF, Heit JA et al. Prevention of venous thromboembolism: the seventh ACCP conference on antithrombotic and thrombolytic therapy. Chest. 2004; 126(suppl 3): 338-400S.
3 Nicolaides A, Fareed J, Kakkar A et al. Prevention and treatment of venous thromboembolism - International Consensus Statement. International Angiology. 2013; 32(2): 111-260.
